Monkeypox Misdiagnosis: Relevant Pox Politics from the Past
In 2011, a young boy in the Congo was misdiagnosed with monkeypox when in fact he has a disease known as “yaws”. Yaws is a form of syphilis. It’s a non-sexually-transmitted syphilitic disease that’s caused by the same species of bacteria that causes syphilis. The bacteria Treponema pallidum subspecies pertenue is the pathogen that causes Yaws. In contrast, the bacteria Treponema pallidum subspecies pallidum is the pathogen that causes the STD known as syphilis. Nonetheless, under a microscope, yaws and the STD syphilis look exactly the same and are totally indistinguishable.Though yaws is caused by the same species of bacteria that causes syphilis, yaws is spread through direct, non-sexual contact. Yaws is spread through skin-to-skin contact with an infected person. So, yaws can spread through casual skin-to-skin contact while syphilis is generally spread through intimate sexual contact only. But interestingly, a document released by the WHO in 1957 talks about how the syphilis bacteria tends to prefer the warmest areas of the body such as the genitals and the armpits and in the same document they describe studies showing that flies were able to transmit the syphilis bacteria from an open wound to a new host (this was an animal study performed on rabbits).
Sexually transmitted diseases (STDs) like syphilis are sometimes used politically as a stigmatizing agent against specific groups of people. Syphilis is not the first STD that I’ve studied that can be transmitted through casual contact. Trichomonas or “Trich” is another STD that can, indeed, be spread through sexual contact, but that can also be spread when people share bath towels or other personal items. It’s important for average people to know that a diagnosis like monkeypox or syphilis could be spread through casual contact.
Not once, but twice as a young adult, a doctor accused of being promiscuous because they believed I had an STD. On one of those occasions, I was in college and I had a fungal infection that developed in my mouth. The doctor accused me of having this STD, but he didn’t know I was a virgin. And I didn’t feel like revealing this information to him (He later misdiagnosed a corneal ulcer and covered my eye with a bandage. I almost went blind as a result). On another occasion, I was married and monogamous and the doctors accused me of cheating a promiscuity, which was totally unfounded, but impossible to prove given their final diagnosis. I had been diagnosed with an STD, not because of lab results, but because, once again, I had a recurring Urinarty Tract Infection that they couldn’t seem to treat. So they finally just decided that it must be an STD and that I must have caught it because I was a promiscuous person.
And on one other occasion, when I was traveling, I visited a doctor in Florida for the UTI problem (again) and he told me this time that my husband was probably cheating on me. He didn’t know that John and I lived in an RV with our 3 year old and that we’d been traveling constantly and moving from one city to the next for nearly a year together. John and I literally spent every moment together, practically in the same room. So I have experience with STDs and how doctors wield them against patients when diagnosing patients becomes too difficult.
But syphilis is a very special disease and it’s been used for centuries to hurt certain groups of people needlessly. The Tuskegee Study enrolled 400 black men with syphilis back in the mid-1930s to study how the disease evolves over time. These men were never told that they had syphilis. Rather, they were told that in exchange for participating in the experiment, they would receive free medical care. They didn’t know that they were purposely being given medicines that would NOT cure their disease so that the United States Public Health Service could “study” the evolution of syphilis. Penicillin was invented and it worked quite well to treat syphilis, but still the Tuskegee Study continued and the men received no penicillin treatments. Indeed, they were given pills that were nothing but placebos. A leak to the press in 1974, finally revealed the study to the public and the men who were still alive were finally able to receive treatment.
So monkeypox raises red flags for me because of the similarities between monkeypox and syphilis. Monkeypox is even being held up by the media as a pseudo-sexually transmitted disease that can also spread casually. There’s something wrong with this presentation of monkeypox because a number of non-STDs can be spread sexually, for example: Ebola, Zika, Dengue. We don’t hold up the sexual transmission of these diseases in the spotlight, though in reality, women especially need to know that they could catch Zika from their partner sexually. So why is monkeypox making the news as an STD (sort of) where we’re talking about gay men instead of just talking about sexual transmission that can happen through any kind of sexual contact, including hetersexual contact?
Monkeypox seems to have the strong stench of a political-disease.
 Click here to subscribe to the Living Database!
Click here to subscribe to the Living Database!
What is Yaws?
Yaws is a tropical disease that usually occurs only in hot, humid areas of the world, but it resembles monkeypox in many ways. Indeed, monkeypox is a disease that scientists have proclaimed to be spread among individuals who have direct, skin-to-skin or intimate sexual contact. Yaws is transmitted through a similar skin-to-skin type of contact that’s very similar to how monkeypox is spread according to the media.Yaws and other versions of syphilis including Bejel and Pinta are spread like monkeypox through skin-to-skin contact. Syphilis is a bacterial disease and monkeypox is said to be a viral disease, but note that syphilis is notoriously hard to see and hard to diagnose through regular lab microscopy. Syphilis infections are caused by a very tiny spirochete bacteria not unlike Helicobacter pylori, the bacteria that causes gastritis and stomach ulcers (as well as GERD, stomach cancer, and other digestive diseases). Indeed, a number of patients with H. pylori infection may actually have syphilis (Treponema pallidum) or both types of infection.
Indeed, some doctors have noted a relationship between syphilis infection and lupus as well as a relationship between H. pylori infection and lupus. Currently, I’m researching syphilis more closely as a possible agent that influences (either directly or indirectly), the development of autoimmune diseases. In reality, most people can cure autoimmune disease using Chlorine Dioxide Solution / Miracle Mineral Solution, but they can only find this information about this medicine if information online is written and organized in a way that they can gain access to it. I regularly see news articles about the syphilis epidemic and how this disease is taking over the world, but patients should know that even drug-resistant syphilis can be treating using Chlorine Dioxide Solution / Miracle Mineral Solution or by using penicillin combined with Dimethylsulfoxide. Dimethylsulfoxide (DMSO) is an FDA-approved medicine that easily combines with most drugs to enhance their effects. Drug-resistant bacteria like MRSA or drug-resistant syphilis become susceptible to antibiotics again when those antibiotics are properly combined with DMSO. And though DMSO is FDA-approved for cystitis in pregnant women (highlighting the low toxicity of this drug), your doctor can combine it with penicillin to enhance its effects if he or she is willing to do so.
 1ness Chlorine Dioxide Kit - Set Hydrochloric Acid 4% (HCl) : Sodium Solution 28% (4 Oz)
1ness Chlorine Dioxide Kit - Set Hydrochloric Acid 4% (HCl) : Sodium Solution 28% (4 Oz)
- Chlorine Dioxide Solution is a reactive oxygen species medicine that is able to cure most infectious diseases including monkeypox, yaws, and syphilis.
- Dimethylsulfoxide (DMSO) can be combined with medicines like penicillin or azithromycin to increase their effectiveness at treating drug-resistant infections like MRSA or drug-resistant syphilis. DMSO is FDA approved, but it is an over-the-counter medicine. Nonetheless, you can talk to your doctor about combining an antibiotic with DMSO to treat drug-resistant bacteria. Note that this type of therapy is widely used in no-chemo/low-chemo cancer treatment facilities to administer tiny doses of chemo. In these setting this therapy is called DMSO-Potentiation Therapy or DPT.
- There are herbal remedies for syphilis that can also be used to cure yaws, bejel, and pinta and that may also be effective as herbal remedies for monkeypox.
 DMSO 8 oz. Glass Bottle Non-diluted 99.995% Low Odor Pharma Grade Liquid
DMSO 8 oz. Glass Bottle Non-diluted 99.995% Low Odor Pharma Grade Liquid
Yaws vs. Monkeypox: What’s the Difference?
Yaws: Basic Information
- Yaws is a tropical infection that occurs in South America, Asia, Oceania, and Africa.
- Yaws affects the skin, bones, and joints.
- Yaws is spread through direct, non-sexual contact with lesions.
- Treatment by conventional medicine doctors typically involves some type of penicillin injection and azythromycin or tetracycline treatments (orally).
Yaws Symptoms
- Yaws Symptoms include the following:
- Round, hard swellings on the skin (2-5 cm) that break open into ulcers, though these swellings vary in size and may not always break open into ulcers
- These swollen ulcerations can take take 3-6 months to heal
- The skin on the soles of the feet and palms of the hands may break open.
- Joint and bone pain
- Fatigue / exhaustion
- Bones may become misshapen.
- Skin necrosis can occur with long-term infection.
Monkeypox Basic Information
According to the WHO, monkeypox is currently the most important orthopoxvirus pertaining to public health. In the media, monkeypox is regularly compared to smallpox, though the two diseases are quite different from each other in terms of severity and mortality rate. Scientists started looking closely at monkeypox about 10-15 years ago.Monkeypox Symptoms
Monkeypox Symptoms include the following:- Blister-like or pimple-like rash that appears on the face and inside the mouth or on other parts of the body including the feet, hands, chest, anus, or genitals.
- The rash can take several weeks to heal.
- Muscle aches
- Backache
- Headache
- Chills
- Extreme fatigue
- Sore throat
- Depression
Resources:

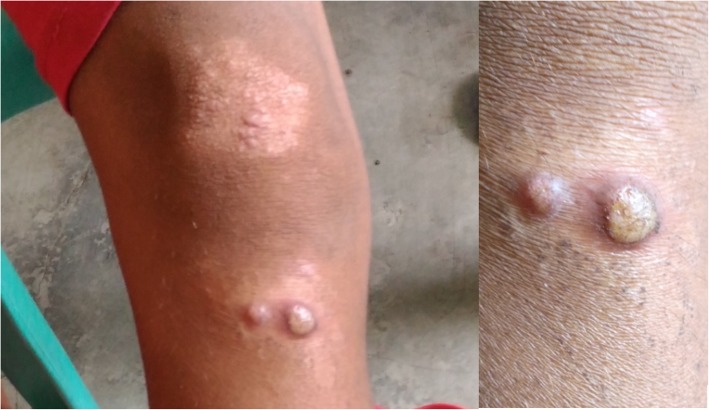 This is an image of Yaws blisters which are strikingly similar to monkeypox except they're caused by the same bacteria that causes syphilis. Note also that the syphilis bacteria is EXTREMELY hard to see through traditional microscopy...and that syphilis has been known for centuries as The Great Imitator of other disease.
This is an image of Yaws blisters which are strikingly similar to monkeypox except they're caused by the same bacteria that causes syphilis. Note also that the syphilis bacteria is EXTREMELY hard to see through traditional microscopy...and that syphilis has been known for centuries as The Great Imitator of other disease.