Prolactin Levels and Depression, Anxiety, and Psychosis
Prolactin is a hormone that is most famous for its role in pregnancy and lactation. But prolactin does many things. It behaves as a neuropeptide that impacts the nervous system in important ways by inhibiting the hypothalamic-pituitary axis too, for example. And prolactin also plays a role in the body’s stress response and in its response to trauma.
In women, prolactin governs parts of the emotional experience associated with motherhood. During pregnancy and lactation, high levels of prolactin (a.k.a. hyperprolactinemia) can be beneficial and natural. There are situations where high levels of prolactin is a positive thing. On the other hand though, hyperprolactinemia can also be associated with endocrine disorders. And during pregnancy and lactation, high prolactin levels, or at least, too few prolactin receptors for the level of prolactin being released in the body has been correlated with mental health issues like anxiety, depression, and even postpartum psychosis. In any case, in some women, the high prolactin levels that occur just prior to milk “let down” can lead to high levels of anxiety.
Not all women experience the release of prolactin as unpleasant during lactation. When women have high levels of anxiety (or depression, or odd, scary thoughts) caused by the release of prolactin during breastfeeding, symptoms are often being caused by exposure to trauma. Most women, after all, experience trauma during childbirth even if the birthing process itself was easy. Trauma, by definition in psychology, is a situation in which a person feels that their life is threatened. By definition, “trauma” is therefore subjective. Trauma can be something very mundane like tripping and falling while crossing the street. Whether a person experiences a situation like falling down in the street as a “trauma” or not, would depend on many factors including the person’s history with tripping and falling and with streets and their sense of what’s happening in the environment around them. But childbirth almost always includes at least one moment, known as “transition” when the baby drops and the woman feels as though she’s going to die. Women who have a C-section also experience this terror when the doctor puts his hands inside her body, creating pressure in the lungs that can make her feel like she’s going to die. Birth, itself, is a situation that causes anxiety for both mothers and fathers because of its high-risk in terms of life and death. So when we talk about prolactin and trauma and postpartum depression, psychosis, or high levels of anxiety, particularly following childbirth when a woman begins breastfeeding, it’s important to acknowledge that women who have been through childbirth have experienced trauma.
Trauma psychology is still in its infancy. Back in the day, scientists referred to trauma using words like “stressors”, which fails to capture the gravity of what trauma can do to both the body and to the mind. So as we begin this discussion about breastfeeding and psychosis as well as postpartum depression or postpartum anxiety, or really any mental health issue that develops after a woman gives birth, we have to also take into consideration the role of trauma.
I’m beginning this discussion of prolactin by pairing the idea of prolactin release and/or uptake with the experience of trauma. There’s a relationship between prolactin levels, release, and uptake and trauma, but this relationship is not extremely straightforward, yet nonetheless, it exists, so we’re going to talk about it. What’s more important though, is for readers to note that for women who are suffering from mental health problems after giving birth, treatment should almost always include treatments that address trauma. Trauma psychology right now is the holy grail in terms of the science of the mind and body and it can explain many things that go wrong in the body or in the mind that seem to have no obvious cause. For example, while some women might develop postpartum depression after giving birth, other women might develop fibromyalgia. So please keep this in mind, as you read about prolactin.
It would be difficult and possibly unwise to target prolactin as an alternative treatment for postpartum psychosis or depression. Prolactin is pretty entwined, physiologically with dopamine and while dopamine lives along a fairly straight-and-narrow highway of precursors and their derivatives that lead from L-phenylalanine to L-tyrosine and L-dopa to dopamine, noradrenaline, and finally adrenaline, prolactin seems to be more centralized (like something at the hub of a wheel) in terms of how it interacts with other neurohormones or neuropeptides. To alter prolactin levels directly could have unpredictable effects on oxytocin, serotonin, or dopamine or other neurotransmitters, but also, research has shown that the body’s and the mind’s response to prolactin levels may have less to do with prolactin itself and more to do with how many prolactin receptors exist to take up the prolactin and use it in a productive way.
In other words, altering the level of prolactin in the body isn’t as likely to impact mental health as altering the number of prolactin receptors in the body. But, if you’re looking for a cure for postpartum depression, anxiety, or psychosis, it might pay off to at least understand a bit about prolactin. High levels of anxiety caused by disturbed prolactin levels and/or too few prolactin receptors can make existing depression, anxiety, or PTSD even worse in the postpartum period. For this reason, it can be valuable for women to know a bit about prolactin and the potential for it to raise anxiety levels briefly (usually in spurts) during lactation. When a woman has experienced trauma, if her body is capped out in terms of how much trauma it can tolerate, the way that the body experiences pleasure can be turned 180 degrees such that pleasurable things become painful. It’s easy for new mothers to misinterpret the feeling of a prolactin release followed by the release of dopamine (and the release of trauma) as the feeling of impending doom in part because, if prolactin release heralds a sense of anxiety due to the woman’s trauma exposure, dopamine can cause that trauma to rise into consciousness for release, which can, in turn, cause women to feel depressed, anxious, or to even have psychotic thoughts.
Don’t misinterpret this information though. Dopamine is the neurotransmitter that normally causes us to feel “parental feelings”. It is the neurotransmitter that makes us able to make decisions and to avoid things that are bad for us and to go toward things that are good for us. Dopamine helps us make positive decisions for our own well-being based on personal experience. But many of us who live in the modern world have had our dopaminergic system hijacked by things like video games, social media, high refined sugar intake, or addictive substances. That’s a strike against our bodies that can make it hard for us to cope with trauma. And if we’ve had traumatic experiences, as all of us have that have not been properly processed by our minds and bodies in a way that allows them to be released, having proper levels of dopamine and the proper number of dopamine receptors to take up the dopamine can lead to a sudden flooding of traumatic material when dopamine receptors regrow. The “flooding” looks a lot like mental illnesses like schizophrenia, depression, anxiety, bipolar disorder, personality disorders, sexual dysfunction, and more. But dopamine itself isn’t bad for us. Rather, if we live our lives with a deficiency of dopamine for a long time, and some of our dopamine receptors die as a result, trauma begins to build up to a critical mass. Either the mind (in the form of mental illness) or the body (in the form of physical illness) will have to “process” this trauma at some point in order to release it. When you have proper levels of dopamine and when dopamine is released regularly in a normal manner, dopamine receptors regrow. This is when the flooding can happen where the mind-body discharges the trauma so that the traumatized person can be healthy again.
But often, in medicine, doctors or psychiatrists, try to close the floodgates on the release of trauma in an effort to cover up symptoms for the person in question when in fact, to close the floodgates can prevent healing.

Click here to buy psilocybin online.
Understanding prolactin and oxytocin and how the body can sometimes respond to the release of their hormones during lactation is a vital piece of information that all women should know about prior to giving birth as prolactin and oxytocin release can, in some, but not all cases, lead to a worsening of postpartum mental illness. Learning a bit about prolactin and oxytocin release and how these hormones can change one’s state of mind during breastfeeding can keep women sane during those first few months of taking care of a newborn infant. Often, in mental illness, it is the body that’s deranged, while the mind is aware that there’s something wrong with how the body feels. Trauma psychology acknowledges that the mind and the body can have these two very different experiences of reality. Anyone who is looking for a cure for postpartum depression, postpartum psychosis, or any kind of mental illness that takes shape in the postpartum period should look closely at Dr. Peter Levine’s work as well as Eye Movement Desensitization and Reprocessing / EMDR, the use of Craniosacral Therapy for postpartum psychosis and depression, among other things. Especially note that sacred medicines like psilocybin mushrooms, Ayahuasca, Iboga, Sapito, Kambo and more can help the body release a lot of trauma quickly. Lydian and I offer a long list of sacred medicines to women during the postpartum period at a small facility just northwest of Mexico City. Contact us at [email protected] for more information about the protocols that we use to treat postpartum psychosis, postpartum depression, and other postpartum mental and physical health issues.
Click here to do a free trial of EMDR online.
Resources:
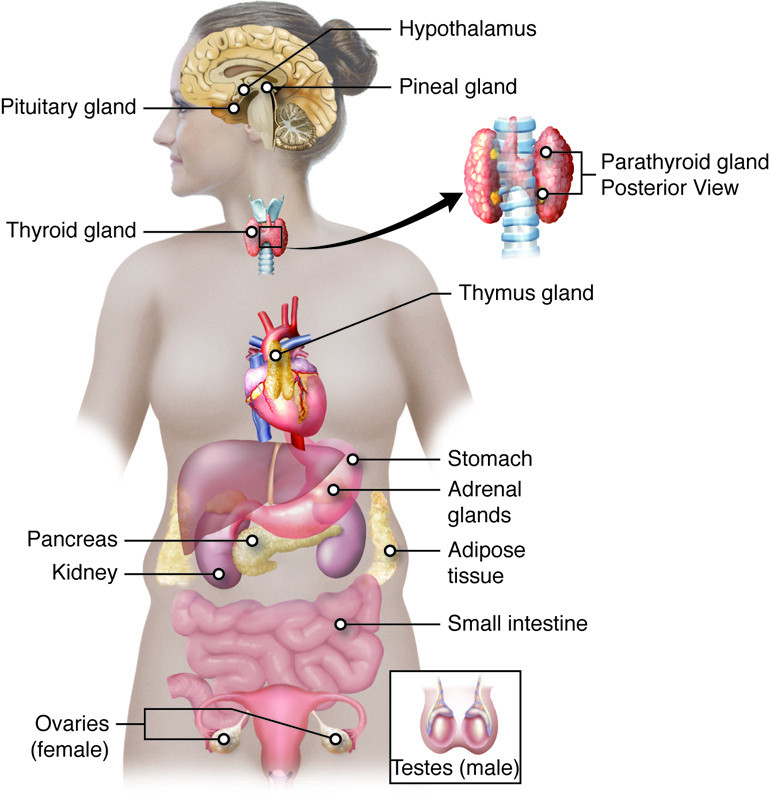
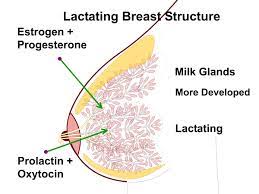 Prolactin plays a role in postpartum depression, postpartum anxiety, and postpartum psychosis, but it isn't super-easy to modify prolactin levels to treat mental health issues. Rather, many women would benefit more from trauma treatments at home to reduce symptoms of postpartum depression, anxiety, or psychosis naturally.
Prolactin plays a role in postpartum depression, postpartum anxiety, and postpartum psychosis, but it isn't super-easy to modify prolactin levels to treat mental health issues. Rather, many women would benefit more from trauma treatments at home to reduce symptoms of postpartum depression, anxiety, or psychosis naturally.