The Fat-Soluble Vitamin Supplement Protocol for Autoimmune Disease
The Fat-Soluble Vitamin Supplement Protocol for Autoimmune Disease
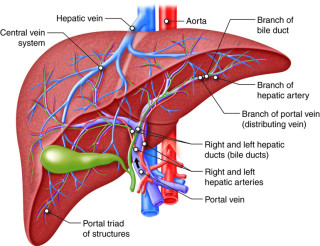
Because patients with autoimmune disease often struggle with liver and gallbladder health, fat-soluble vitamin deficiency can be an issue. This is because bile is essential for the digestion of fats, and therefore also for the digestion of fat-soluble vitamins and other nutrients (such as omega-3 fatty acids). If the liver has trouble producing high-quality bile, or if bile flow is somehow impeded in the gallbladder, then fat absorption will be impaired. This can lead to the development of fat-soluble vitamin deficiencies over time, especially if the person’s diet is poor or less-than-adequate.
Fats and oils are electrical substances and some fat-soluble vitamins like vitamin K1 and vitamin K2 are notably electrical as quinones. Vitamin K1, also known as Phylloquinone, is a major component in chlorophyll, the substance in plants that has the ability to transform carbon dioxide and sunlight photons into energy that the plant uses to survive. Vitamin K2, also known as Menaquinone, plays a vital role in calcium metabolism which impacts both bones and nervous system tissues. Quinones are also essential in the production of catecholamine neurotransmitters like dopamine, noradrenaline, and adrenaline which are often involved in the pathogenesis of autoimmune disease.
Vitamin K2
Some fat-soluble vitamins like vitamin K2, are deficient in most diets, regardless of the person’s attention to eating healthfully. These fat-soluble nutrients must be supplemented due to their lack of presence in the food supply.Vitamin K2 is an essential supplement for any individual with autoimmune disease. This nutrient is severely deficient (if not entirely nonexistent) in most modern food supplies, meaning that diseases caused by its deficiency are remarkably common. Vitamin K2 is found in the highest quantities in animal foods, including red meats, milks, eggs, or poultry, that are organic and grass-fed/free-range, though it’s found in smaller quantities in other fermented foods like organic, unpasteurized sauerkraut and Japanese Natto. Notably, the vast majority of people in developed countries especially are unlikely to eat any of these foods with any sort of regularity. The production of vitamin K2 does not happen in GMO plants. And animals that are given drugs that contain organophosphates do not have vitamin K2 in their gut bacteria which means that they don’t have vitamin K2 in the animal products that they provide to us.
Some of the youngest generations on the planet right now have never eaten these vitamin K2-containing foods at all, and are therefore more likely to be severely deficient in this nutrient.
Vitamin K2 works together with vitamin D to ensure that the calcium we eat ends up in our bones and teeth, and not in the soft tissues of our bodies. Without vitamin K2, much of the calcium we consume gets assimilated into organs and other tissues, resulting in calcifications and other issues like gallstones and kidney stones. But vitamin K2 deficiency not only leads to calcifications, but can also lead to hypercalcemia, or calcium toxicity in the blood (read more about the symptoms of calcium toxicity here).
Calcium toxicity then, in turn, inhibits iodine absorption and further aggravates iodine deficiency. Iodine is another essential nutrient that’s in woefully low supply in the US and that also, notably, is most present in organic, grass-fed/free-range animal products. So, in this way, a vitamin K2 deficiency can actually cause an iodine deficiency, even if the person didn’t already have a deficiency in this mineral beforehand. We talk more about iodine deficiency and autoimmune disease here.
Because vitamin K2 doesn’t exist in the food supply (at least not unless you can get some grass-fed, organic animal protein), and because certain environmental factors such as the ubiquitous presence of organophosphates make hypercalcemia more likely than normal, vitamin K2 supplements are absolutely essential for health. Vitamin K2 supplements can reverse existing calcifications, as well as prevent future ones from occurring. Some of the autoimmune diseases and/or health issues related to autoimmune disease that are known to be related to vitamin K2 deficiency include:
- Dermatomyositis
- Cancer
- Multiple sclerosis (this is specifically correlated with pineal gland calcification)
- Arthritis
- Type 1 diabetes
- Autoimmune diseases involving calcification, which may include:
- Systemic sclerosis
- Systemic lupus erythematosus
- Mixed connective tissue disease
- Scleroderma
- Ankylosing spondylitis
- Sarcoidosis
Vitamin K2 is also an important antidote to organophosphate poisoning. Organophosphate exposure is implicated in a fairly long list of autoimmune conditions, including rheumatoid arthritis, lupus, autoimmune hepatitis, and autoimmune thyroid disease (you can read more about organophosphates and autoimmune disease here).
Autoimmune disease patients should take vitamin K2 in its MK-7 form, which is its natural form. At first, choose a supplement that supplies exclusively vitamin K2 as MK-7. Later, you may use a supplement that contains both vitamin K2 and D3, if you wish (note, though, that you should never take a vitamin D3 supplement on its own; vitamin D3 should always be taken with vitamin K2). This vitamin K2 supplement should be a part of your long-term supplementation protocol, even after you regain your health.
Try to seek out grass-fed/free-range sources of animal protein whenever possible. These foods will contain vitamin K2, as well as iodine, and are also less likely to contain harmful chemicals and other toxins. Free-range poultry and eggs, and grass-fed, organic goat products, may be easier to find than certain other types of meat or milk, though all are permitted on the Autoimmune Disease Diet in moderation, so long as they are grass-fed/free-range and organic.
Vitamin D and Autoimmune Disease
While I don’t deny that vitamin D is absolutely essential for human health, we’re against vitamin D supplementation when it isn’t combined with vitamin K2 except in very rare situations. There are rare cases where vitamin D supplementation is legitimate and valuable, this is true, but for most of the people reading this, vitamin D supplements are likely to do more harm than good. I’m including this section because there’s a lot of misinformation about vitamin D and autoimmune disease on the internet, and I want to offer some clearer information and alternative healthy options to vitamin D supplements.True vitamin D deficiency really only develops in individuals who are exposed to very little sunlight and/or who do not get any vitamin D from their diet. People in northern climates who eat plenty of fish are less likely to develop vitamin D deficiency because these fish tend to have higher levels of the dietary form of vitamin D (even though these people may get little to no sunlight for large portions of the year). And, people who live in other areas, unless they never go out in the sun, are also likely to get sufficient levels of vitamin D from the combination of sunlight exposure and diet.
Finally, let’s not forget the (somewhat excessive) fortification of foods with vitamin D.
In other words, becoming deficient in vitamin D would be difficult. In fact, given the more serious problem of vitamin K2 deficiency, vitamin D is actually more likely to be present in higher-than-normal quantities in some people’s diets. Even foods that are naturally high in dietary vitamin D, like commercial cow’s milk, are often fortified with additional vitamin D.
Read more about the negative effects of vitamin D supplementation without vitamin K2 here.
People who are concerned about their vitamin D intake would do better to take cod liver oil each day. This is a natural, dietary source of vitamin D, and includes other fat-soluble vitamins as well as omega-3 fatty acids. It may also contain vitamin K2 (this is my guess, though it seems that research is lacking on this subject). As such, cod liver oil is a significantly more balanced supplement for general health and healing for autoimmune disease patients. Another way to boost vitamin D levels naturally (and without aggravating vitamin K2 or iodine deficiencies) is to take the Budwig Smoothie daily while sitting out in the sun. If the Budwig Smoothie is made with grass-fed, organic cottage cheese, this recipe also supplies vitamin K2 and iodine, while the sunlight exposure makes it possible for your skin to start the process of producing vitamin D. The Budwig Smoothie also has other valuable benefits for autoimmune disease patients.
Beta-Carotene
Beta-carotene is a natural form of vitamin A. Technically, beta-carotene (and other carotenoids) is a precursor to vitamin A; it must be converted to vitamin A in the body before it can be used. This makes beta-carotene a safer supplement, since there’s less risk of toxicity. With vitamin A supplements like retinol, it’s much easier to “overdose” since this form is the active form of vitamin A. Excess beta-carotene, however, will simply be removed in the urine, similar to a water-soluble B vitamin.VItamin A and beta-carotene have been studied in regard to their benefits in patients with the following types of autoimmune disease:
- Multiple sclerosis
- Diabetes
- Autoimmune encephalomyelitis
- Systemic lupus erythematosus
- Autoimmune hepatitis
Patients with autoimmune disease should supplement with 25,000IU of beta-carotene in addition to eating small amounts of high quality animal proteins, such as free-range, organic eggs, chicken, and grass-fed butter. These animal proteins will contain the active form of vitamin A known as retinol. Individuals who are particularly concerned about vitamin A deficiency could also include a grass-fed liver supplement (or, if you have access to it and are willing to eat it, fresh, grass-fed liver cooked to your liking). Cod liver oil also contains vitamin A in higher quantities. Because some research indicates that some autoimmune disease patients, such as those with hypothyroidism, may have trouble converting beta-carotene to retinol, this balance between supplements and dietary vitamin A sources ensures that your body will get sufficient amounts of vitamin A without risking vitamin A toxicity.
Vitamin E
Vitamin E is a known anti-inflammatory, and is also a powerful antioxidant that can help prevent the oxidation of the B-complex vitamins and vitamin C. This vitamin is also helpful for the absorption of selenium, and is in fact absolutely essential in order for the body to be able to use and store vitamin A. Vitamin E deficiency can also inhibit iron absorption and hemoglobin formation and thus may contribute to iron deficiency anemia over time. So, vitamin E is an important nutrient for autoimmune disease patients looking to improve their overall nutritional profile.Vitamin E has been studied as a treatment or method of management for the following autoimmune diseases:
- Chronic discoid lupus erythematosus
- Rheumatoid arthritis (vitamin E found in fish oil is particularly beneficial for RA patients)
- Autoimmune encephalomyelitis
- Guillain-Barre syndrome (GBS)
- Multiple sclerosis
- Autoimmune neuritis
- Diabetes
Vitamin E can be taken in the form of cod liver oil, which I talk about more below, or it can be taken as its own dedicated supplement (if you’d like, you can take vitamin E and cod liver oil). If you take a vitamin E supplement, be sure to get one that contains d-alpha tocopherol, since this is the safe, natural form of the vitamin. Note that the synthetic form of vitamin E, dL-alpha tocopherol, looks remarkably similar, so make sure to double check the ingredients of your supplement. The maximum daily dose of vitamin E is 800 IU or 540 mg per day; start with half of this at 400 IU per day, especially if you’re also taking cod liver oil or eating the Budwig Smoothie (which is also rich in vitamin E).
Cod Liver Oil
Cod liver oil is a beneficial supplement for patients with autoimmune disease because it supplies most of the fat-soluble vitamins in a bioavailable manner. In addition, it also contains DHA (docosahexaenoic acid) and EPA (eicosapentaenoic acid), two types of omega-3 fatty acids that are known to help reduce inflammation and support healthy brain and nervous system function. Cod liver oil has specifically been studied in regard to its benefits in the treatment of:- Rheumatoid arthritis and other arthritic conditions
- Gastric ulcers (including those perhaps caused by H. pylori, a bacterial infection implicated in a long list of autoimmune diseases)
- Diabetes
- Hashimoto’s thyroiditis
- Ulcerative colitis
- Crohn’s disease
- Psoriasis
- Lupus erythematosus
- Multiple sclerosis
Cod liver oil is a unique supplement in that it contains a well-balanced proportion of various essential fat-soluble nutrients. It contains naturally high levels of vitamin A, vitamin D, and vitamin E; while we don’t recommend taking a vitamin D supplement (unless it’s a combined vitamin K2+D3 supplement), the natural form of vitamin D in cod liver oil can be a safe and healthy way to add in a little extra of this nutrient to your diet.
Cod liver oil also may benefit autoimmune disease patients by reducing pain (through its anti-inflammatory properties), alleviating depression and anxiety, healing all manners of skin problems, and supporting general cardiovascular health. This supplement has also been shown to help improve adrenal imbalances and may relieve adrenal fatigue. Cod liver oil is available in gel capsule form or as an actual oil that you can drink. Some people may prefer the gel capsules, but keep in mind that the actual oil is more likely to be effective (Dr. Weston Price recommended combining the oil with a vitamin K2-rich butter for maximum benefits). Take 2 teaspoons of regular cod liver oil daily, or 1 teaspoon of high vitamin cod liver oil per day. Women who are pregnant or nursing should take double this dose, while children ages 3 months to 12 years should take half of this dose.
Some cod liver oils are lemon-flavored, and have very little fishy taste at all. Personally, I don’t like fish at all, but I’ve never had a problem drinking a spoonful or capful of lemon-flavored cod liver oil. In fact, I think it has a pleasant flavor. You can take this oil straight, or you can mix it into a salad dressing or smoothie, the choice is yours. If you’re taking the Budwig Smoothie daily, it could be mixed into this after the initial quark-flax oil blending as well.
 NOW Supplements, Cod Liver Oil 650 mg, Excellent Source of Vitamins A and D-3, 250 Softgels
NOW Supplements, Cod Liver Oil 650 mg, Excellent Source of Vitamins A and D-3, 250 Softgels
A Note on Fat-Soluble Vitamins and Autoimmune Disease…
Large bodies of research exist to support the idea that patients with autoimmune disease tend to be deficient in one or more of the fat soluble vitamins (these are vitamins A, D, E, K1, and K2). This makes sense to us, since many autoimmune disease patients also tend to struggle with liver and gallbladder health. Bile, which is produced by the liver and stored and released by the gallbladder, is absolutely essential for the digestion of fats, and therefore also for the digestion and absorption of fat soluble vitamins. If something goes wrong with the liver or gallbladder, the absorption of fats, and the nutrients inside these fats, is also likely to be impaired. Over time, this can indeed lead to a deficiency in one or more fat soluble nutrients.Note that a buildup of biliverdin (which is green) or bilirubin in the skin happens when the liver or gallbladder is having trouble detoxifying themselves. Exposure to complementary light colors (red light for green biliverdin tones and ultraviolet / blue light for yellow bilirubin tones) can help the skin, liver, and gallbladder detoxify more quickly. Exposure to the complementary color of light (depending on the patient’s skin hue) or exposure to full-spectrum light of the sun charges the non-polarized molecules of biliverdin or bilirubin so that they can be more easily removed from the body.
We also recommend taking an ox bile supplement and pancreatic enzymes with every meal, especially meals that have a high fat content. Ox bile supplements help digest fats and thus encourage the absorption of the nutrients in fats. It also seems logical to recommend that patients take ox bile and pancreatic enzymes when they take their fat-soluble supplements, since without these additional supplements, autoimmune disease patients may struggle to actually absorb these vitamins and other nutrients effectively until they’re able to fully heal their liver and gallbladder.
Plan ahead to take ox bile, pancreatic enzymes, cod liver oil, vitamin K2, and your other fat-based supplements with meals for best results.
Read more about ox bile supplements here.
Learn about pancreatic enzyme therapy here.

The Barefoot Healer's Guide to Autoimmune Disease, Volume 1 - BUY HERE!
 Click here to subscribe to the Living Database!
Click here to subscribe to the Living Database!
Related Posts: https://alivenhealthy.com/2023/01/09/diet-protocols-for-autoimmune-disease-patients-the-budwig-diet-the-gerson-protocol-and-more-to-cure-autoimmunity/ https://alivenhealthy.com/2022/06/04/how-to-use-enzyme-therapy-for-better-digestion-to-prevent-cancer-cure-autoimmune-disease-and-reclaim-your-health/ https://alivenhealthy.com/2023/01/11/can-diet-cure-autoimmune-disease-vitamin-b17-amygdalin-and-other-nutrient-cures-for-autoimmunity/ https://alivenhealthy.com/2023/01/09/the-autoimmune-disease-diet-the-basic-guidelines-for-healthy-eating/ https://alivenhealthy.com/2022/12/27/alternative-treatment-for-autoimmune-disease-high-dose-vitamin-c-therapy/ https://alivenhealthy.com/2023/01/09/the-autoimmune-diet-what-to-eat-and-what-foods-to-avoid-to-increase-health-and-healing/ https://alivenhealthy.com/2023/01/06/toxic-load-and-autoimmune-disease-how-pharmaceutical-drugs-and-environmental-toxins-cause-autoimmunity/ https://alivenhealthy.com/2023/01/03/how-vitamin-b-complex-deficiency-causes-autoimmune-disease/ https://alivenhealthy.com/2022/11/20/everything-you-need-to-know-about-vitamin-k2/ https://alivenhealthy.com/2022/05/19/vitamin-d-harmful-effects-of-supplementing-without-vitamin-k2/ https://alivenhealthy.com/2019/05/13/vitamin-a-cancer-therapy/
Resources:

 Bronson Vitamin K2 (MK7) with D3 Supplement Bone and Heart Health Non-GMO Formula 5000 IU Vitamin D3 & 90 mcg Vitamin K2 MK-7 Easy to Swallow Vitamin D & K Complex, 250 Capsules
Bronson Vitamin K2 (MK7) with D3 Supplement Bone and Heart Health Non-GMO Formula 5000 IU Vitamin D3 & 90 mcg Vitamin K2 MK-7 Easy to Swallow Vitamin D & K Complex, 250 Capsules
 4th & Heart Original Grass-Fed Ghee, 16 Ounce, Keto, Pasture Raised, Non-GMO, Lactose and Casein Free, Certified Paleo
4th & Heart Original Grass-Fed Ghee, 16 Ounce, Keto, Pasture Raised, Non-GMO, Lactose and Casein Free, Certified Paleo
 Barlean's Organic Flaxseed Oil Liquid, Cold Press Flax Seeds, 7,640mg ALA Omega 3 Fatty Acid Supplement for Joint and Heart Health & Healthy Digestion, 32 oz
Barlean's Organic Flaxseed Oil Liquid, Cold Press Flax Seeds, 7,640mg ALA Omega 3 Fatty Acid Supplement for Joint and Heart Health & Healthy Digestion, 32 oz
 Swanson Beta-Carotene Vitamin A 25000 IU Skin Eye Immune System Health Antioxidant Support 7500 mcg 300 Softgels Count
Swanson Beta-Carotene Vitamin A 25000 IU Skin Eye Immune System Health Antioxidant Support 7500 mcg 300 Softgels Count
 Solgar Vitamin E 268 MG (400 IU) (d-Alpha Tocopherol & Mixed Tocopherols), 100 Softgels - Supports Immune System & Skin Nutrition - Natural Antioxidant - Gluten Free, Dairy Free - 100 Servings
Solgar Vitamin E 268 MG (400 IU) (d-Alpha Tocopherol & Mixed Tocopherols), 100 Softgels - Supports Immune System & Skin Nutrition - Natural Antioxidant - Gluten Free, Dairy Free - 100 Servings
 Carlson - Cod Liver Oil, 1100 mg Omega-3s, Liquid Fish Oil Supplement, Wild-Caught Norwegian Arctic, Sustainably Sourced Nordic Liquid, Lemon, 250 ml
Carlson - Cod Liver Oil, 1100 mg Omega-3s, Liquid Fish Oil Supplement, Wild-Caught Norwegian Arctic, Sustainably Sourced Nordic Liquid, Lemon, 250 ml
 Vital Nutrients Pancreatin and Ox Bile Extract | Natural Digestive Enzyme Supplement | Helps Break Down Protein, Fat, and Carbs* | Gluten, Dairy and Soy Free | 60 Capsules
Vital Nutrients Pancreatin and Ox Bile Extract | Natural Digestive Enzyme Supplement | Helps Break Down Protein, Fat, and Carbs* | Gluten, Dairy and Soy Free | 60 Capsules