What is hyperprolactinemia?
Hyperprolactinemia is defined as an elevated level of the hormone prolactin in the blood. It is a common endocrine imbalance that is observed more often in women than in men. It’s caused by pregnancy, chronic stress, excessive physical activity, and sometimes by pituitary adenoma (a type of cancer on the pituitary gland). If you have been diagnosed with hyperprolactinemia caused by a prolactinoma tumor, be sure to read about cures for cancer in our Cancer Cure Catalog books or do some of our online cancer cure video courses that discuss the same material. Be sure to look closely at Lugol’s iodine and frankincense plus dimethylsulfoxide / DMSO for cancer treatment if you have a pituitary tumor that is causing hyperprolactinemia.Hyperprolactinemia is, unfortunately, an under-discussed health problem, especially when it comes to natural treatments and therapies for chronic pain. It can affect both men and women, though it most frequently affects women, especially women who have another co-existing reproductive hormone imbalance caused by a disorder such as PCOS (to name just one of these disorders). This article will focus primarily on hyperprolactinemia in women, but we’ll also talk about hyperprolactinemia in men, and treatments for both genders as this is a problem involving hormone imbalance which is not a gender-specific issue.
As its name suggests, hyperprolactinemia is a condition characterized by abnormally high levels of prolactin. Prolactin is a hormone that is not only responsible for breast development and breastmilk production, but also for other lesser-known functions, including regulation of the immune response. As we’ve already discussed earlier, it can be valuable to think of the immune system as one of the three parts of a system that also includes the autonomic nervous system and the endocrine system.
Prolactin may also play an important role in liver health and function, since the liver is one of the primary locations in the body where there are prolactin receptors (along with the gonads, of course, and the lymphoid cells in the lymphatic system). This would make some sense, since the liver is one of the main organs of the body that produces and processes certain hormones and nutrients that are necessary for hormone creation. It is also an organ that is often involved in producing pain in the body.
With that in mind, let’s orient toward prolactin in terms of chronic pain to see what this model can teach us.

Click here to schedule a health coaching call with us.
Symptoms of Hyperprolactinemia
The symptoms of hyperprolactinemia include:- Estrogen deficiency (symptoms of estrogen deficiency are below)
- Pain during sexual intercourse due to lack of vaginal lubrication
- Higher incidence of urinary tract infection (UTI)
- Absence of menstruation / Amenorrhea
- Mood swings
- Tender breasts
- Hot flashes
- Fatigue
- Difficulty concentrating
- Depression
- Headaches and/or migraines
- Progesterone deficiency (symptoms of progesterone deficiency are below)
- Menstrual irregularities
- Heavy menstruation
- PMS / Premenstrual Syndrome
- PMDD / Premenstrual Dysphoric Disorder
- Tender breasts
- Bloating / swelling
- Painful menstruation / Dysmenorrhea
- Ovarian cysts
- Recurrent miscarriage
- Insomnia
- Weight gain
- Mood swings
- Constipation
- Headaches and/or migraines
- Testosterone deficiency (symptoms of testosterone deficiency are below; this symptom may occur in both men and women)
- Decreased energy
- Low libido
- Trouble concentrating
- Erectile dysfunction (in men)
- Loss of lean muscle
- Anovulatory infertility
- Irregular menstruation
- Heavy periods
- Galactorrhea (spontaneous breast milk production outside of pregnancy or the postpartum period when a woman is breastfeeding; may occur in both women and men)
- Breast pain (may occur in both women and men)
- Low libido (may occur in both women and men)
High levels of prolactin are known to interfere with the release of Gonadotropin Releasing Hormone (GnRH) from the hypothalamus. This hormone is responsible for directing the release of luteinizing hormone and follicle stimulating hormone, which in turn are responsible for producing estrogen and progesterone (as well as testosterone, though somewhat indirectly). So, in this way, increased prolactin can interfere with the levels of other better-known human reproductive hormones.
 The Natural Women's Health Guide, Volume 2 - Fertility, Natural Fertility Enhancers, Infertility Treatments, and Natural Libido Boosters - BUY HERE!
The Natural Women's Health Guide, Volume 2 - Fertility, Natural Fertility Enhancers, Infertility Treatments, and Natural Libido Boosters - BUY HERE!
What causes hyperprolactinemia?
Hyperprolactinemia may be caused by a variety of issues, including those listed below:- Prolactinoma (this is a tumor of the pituitary gland, and is ultimately the cause for up to 50% of hyperprolactinemia cases)
- Hypothyroidism / Poor thyroid function
- Chronic kidney disease
- Chronic liver disease
- Recent injuries/points of trauma to the upper chest area (this may include surgeries or injuries to the rib cage, diaphragm, upper abdomen, and some infections like Herpes zoster / Shingles)
- Use of certain pharmaceutical drugs (opiates, SSRI antidepressants, GERD medications, antipsychotics, and medications for ulcers of the digestive tract)
- Synthetic estrogen treatments (such as those given at menopause)
Hyperprolactinemia and Chronic Pain Conditions
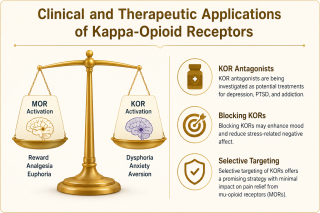
There are a variety of chronic pain conditions that are caused by hyperprolactinemia. Some scientists have speculated that higher levels of prolactin in women may contribute to the higher incidence of chronic pain in women, but it seems unlikely that this is the whole story. Studies have shown that high levels of prolactin can sensitize the nociceptive receptors differently in women than in men which is thought provoking and worth consideration though. In our experience, the relationship between hyperprolactinemia and chronic pain might be mediated through childbirth and breastfeeding including trauma-based physiological reactions like Dysphoric Milk Ejection Reflex (D-MER). D-MER is a condition that affects women when they’re lactating. It involves a sudden feeling of dread or doom, anxiety, sadness, or even anger just before milk let-down. The feelings are intense and like other trauma-based feelings, they don’t follow the normal arc of human emotions where they blend with present-tense reality, plateau and then release. These trauma-based D-MER feelings feel like they could last forever (though they never do) and because they’re associated with breastfeeding, they can affect the mother-child bond. D-MER involves a rapid drop in dopamine levels. Prolactin spurs the production of milk, but oxytocin triggers the release of milk from the breasts, the so-called “let-down”. Scientists believe that there is an inverse relationship between dopamine and prolactin where the abrupt reduction in dopamine accompanies an abrupt increase in prolactin that is too fast or too large such that the dopamine deficit leads to dysphoria and the strong negative emotions. Though the kappa-opioid receptors have not specifically been studied in relation to D-MER, it warrants mentioning that the kappa-opioid receptors are often involved in dysphoric states and they are likely involved in D-MER as well. D-MER has been correlated with nipple nerve pain and other forms of neuropathy in the body, but what’s interesting is that some women develop dysphoria and experience negative emotional states (essentially trauma-based flashbacks) that are triggers by milk let-down while other women develop neuropathy. This suggests that some women feel their negative trauma-based emotions while other women transmute these emotions into physical pain. Needless to say, some of the chronic pain conditions that are impacted by prolactin include:- Fibromyalgia
- Migraine headaches
- Pelvic pain
- Gout
- Arthritis
- Rheumatic diseases
- Lupus
- Sjogren syndrome
- Systemic sclerosis
- Autoimmune disorders involving chronic pain
- Complex regional pain syndrome / CRPS
Conventional Medications for Hyperprolactinemia
Normally, I don’t talk about the conventional prescription medications for diseases. But in this case, I thought it was necessary, since the drug that’s generally given to hyperprolactinemia patients may actually worsen their condition considerably. There are a few different drugs that may be prescribed for hyperprolactinemia, but one of the most commonly prescribed is Bromocriptine (brand names: Parlodel; Cycloset). Bromocriptine is a dopamine receptor agonist that contains bromine, a halogen element that competes with iodine in the body’s iodine receptor sites in the thyroid, reproductive organs, gallbladder, and beyond.Bromine / bromide toxicity is already a major problem in many developed countries, since it’s present in drinking/bathing water, in pajamas and clothes, on furniture, in swimming pools, and even sometimes in the air in the form of certain pesticides like Naled. Exposure to bromine / bromide not only causes the symptoms of bromine toxicity (you can read more about these here), but also causes and/or aggravates iodine deficiency.
Many cough medications contain bromine / bromide as an excipient even though potassium iodide is a healthy and very effective expectorant that won’t make you sicker. This is relevant when we talk about chronic pain because one of the cough suppressants, dextromethorphan, has been used to effectively reduce fibromyalgia pain. Unfortunately though, most dextromethorphan formulations contain bromine / bromide. If you can find dextromethorphan hydrochloride however (which substitutes chloride, an electrolytes our bodies need, for the bromide), this medicine can be useful in getting rid of fibromyalgia or rheumatic pain.

Click here to learn more and download the Living Database now.
Bromocriptine Side Effects / Why You Should Avoid Bromocriptine
Bromine / bromide exposure is serious. Many insecticides contain bromine / bromide because this substance hijacks the nervous system. Indeed, the role of bromine / bromide in the nervous system really highlights what iodine does to heal the nervous system. Iodine deficiency is a serious problem for babies and children during pregnancy, lactation, and beyond as it contributes to learning problems and cognitive issues. Fetuses, babies, and children need plenty of iodine in order to be healthy on all levels, but in young children, iodine can make or break nervous system development. As such, it’s important to be aware of bromine / bromide in the environment, in foods, as excipients in medications, and in the air we breathe (as it is used as an insecticide on agricultural crops). Bromocriptine for hyperprolactinemia will initially improve symptoms, but later begin producing new and more serious symptoms of disease when the body hits critical mass in terms of the bromine / bromide. Some of the side effects of Bromocriptine include (but are not limited to):- Nausea
- Hypotension / low blood pressure
- Dizziness
- Loss of appetite
- Visual hallucinations
- Heart palpitations
- Vertigo
- Nightmares
- Constipation
- Difficulty swallowing (this is actually likely due to swelling of the thyroid gland in response to bromine toxicity/iodine deficiency)
- Seizures
- Fatigue
- Skin rash / hives
- Internal bleeding
- Loss of coordination
- Heart attack
- Psychosis
Treatments for Hyperprolactinemia
Prolactin has an important and pronounced effect on the menstrual cycle in women which is, perhaps, why hyperprolactinemia might be observed more often in women than in men. It’s possible that hyperprolactinemia is just as common in men, but its effects are less obvious or less distressing. In any case, dopamine plays an important role inhibiting prolactin production and secretion. We’ve already talked about one of the roles that dopamine plays in terms of histamine and chronic pain in an earlier discussion about histamine. Dopamine is the primary neurohormone for left-brain, logical thinking and decision making. When dopamine levels get low, a person becomes susceptible to addiction and addictive behaviors because we use dopamine as fuel to make decisions for ourselves based on our prior experiences and how those experiences panned out for us. Addictive behaviors are rooted in trauma and an inability to access or use left-brain, logical information about our past experiences with an addictive behavior to stop doing something that’s harming us. In any case, beyond the emotional-behavioral aspects of what dopamine does in the body, this neurohormone is also the precursor substance for noradrenaline (another neurohormone that factors hugely into autonomic nervous system function) and adrenaline, the so-called fight-or-flight hormone that manages our sympathetic nervous system response. Dopamine also inhibits prolactin synthesis and secretion to essentially reduce prolactin levels that are too high.So dopamine is an important neurohormone in chronic pain and it’s important that you have enough of this substance in your body. Bromocriptine, in fact, is said to reduce prolactin through its impact on dopamine, albeit with severe side effects and eventual bromine toxicity in the patient’s future.
Below we’ll talk about herbs that increase dopamine levels in a big way as well as herbs that balance prolactin levels through other mechanisms of action.
Bitter Kola Nut (Garcinia Kola / Cola accuminata)
Garcinia kola was once an important medicinal ingredient in Coca Cola. Today, of course, Coca Cola is far from being a medicine, but back when it was first developed, Coca Cola was a nerve tonic that had been developed to reduce pain and inflammation while improving energy levels.
Click here to buy Bitter Kola Nut.
The bitter kola nut is used in traditional African medicine as an herbal remedy for chronic pain and other conditions that involve a number of serious health problems. The bitter kola nut is a powerful and intelligent hormone-balancing treatment that will raise hormone levels, if needed, or lower them if that would better serve a person’s physiology. Its effects on prolactin levels in both men and women depend on what the person’s physiology demands in order to produce balance. It is through this mechanism of action, that Garcinia kola works on many chronic pain conditions.
Click here to buy The Home Brewed Ko-Ka-Ko-La Cure.
Vitex Berry / Chaste Berry (Vitex agnus-castus)
For women, vitex berry (Vitex agnus-castus) is an important herbal remedy for hyperprolactinemia. This herb can help balance prolactin levels, as well as levels of all of the other reproductive hormones, and is indicated as one of the most important herbs for women’s health during the reproductive years (though vitex berry may also prove beneficial for post-menopausal women with hyperprolactinemia).Studies have shown that even low-dose vitex berry can be highly effective in the treatment of hyperprolactinemia in women. One study observed that a dose of 40 mg of vitex berry, given 3 times daily successfully lowered prolactin levels and relieved the symptoms of mastalgia (breast and nipple pain) to an equal extent as bromocriptine, but without any side effects.
A different study on a group of 52 women with hyperprolactinemia, the administration of 20 mg of vitex berry for 3 months reduced prolactin release, rebalanced luteal phase progesterone synthesis and release, and shortened the length of the women’s luteal phase. Yet another study suggested that the vitex berry given at a dose of 30-40 mg/day was able to reduce abnormally high levels of prolactin by 80%, in addition to helping resolve other symptoms of hyperprolactinemia, such as amenorrhea, oligomenorrhea, menorrhagia, polymenorrhea, problems with the function of the corpus luteum, and cystic hyperplasia. Multiple studies also indicate that women with hyperprolactinemia who are trying to conceive are more likely to get pregnant when they take vitex berry in the months prior to conception than other women with hyperprolactinemia who are not taking this herbal supplement.
The plant’s ability to lower prolactin levels may be due to its dopamine receptor agonist activity in the brain; note that the vast majority of drugs that are prescribed for hyperprolactinemia are also dopamine receptor agonists, so vitex berry may work as a kind of herbal substitute for these pharmaceutical drugs. As a bonus, vitex berry carries little to no risk of side effects, and can be taken over the long term. Women who become pregnant can take the herb for the 1st trimester in order to prevent miscarriage, and then stop taking it for the rest of the pregnancy. Since hyperprolactinemia often occurs in combination with Polycystic Ovarian Syndrome / PCOS, it’s worth mentioning that vitex berry has also been shown to help increase progesterone and estrogen levels, decrease testosterone levels, and reduce the number of ovarian cysts present in women with polycystic ovarian syndrome.
 Click here to buy Vitex Berry.
Click here to buy Vitex Berry.
Velvet Bean / Mucuna (Mucuna pruriens)
Mucuna pruriens contains high levels of L-dopa, the natural amino acid precursor to the neurotransmitter dopamine (as differentiated from the pharmaceutical drug known as L-dopa which is a completely different substance that can harm the body). As such, Mucuna is frequently used as a treatment for problems like addiction, Alzheimer’s disease, depression/anxiety, and other mental health disorders. The presence of L-dopa in Mucuna pruriens also happens to make it a candidate for the treatment of hyperprolactinemia in both women and men. Indeed, studies have proven that this particular herb, through its dopamine-increasing action, can lower abnormally high prolactin levels.

Click here to buy The Mucuna Pruriens Protocol book.
Mucuna pruriens has a mild contraceptive effect in women, as well as a simultaneous fertility boosting effect in the rebound period after the woman stops taking it. Women taking Mucuna pruriens for hyperprolactinemia should be aware of this, but should also know that Mucuna doesn’t prevent conception in all cases, and can increase fertility when used at the appropriate times in a woman’s menstrual cycle. If, however, you become pregnant while using Mucuna as a hyperprolactinemia treatment, stop taking the herb until after birth (and then, be aware that Mucuna can interfere with breast milk supply, so be prepared to stop taking it until you stop breastfeeding, if needed). Its effect on breast milk supply is through its ability to inhibit prolactin production and release, of course, a desirable effect for a woman with D-MER. In men, Mucuna pruriens generally increases fertility. You can read more about Mucuna’s effects in both men and women here.
Click here to learn about Mucuna pruriens by doing an online Video Course.
Take a dose of up to 6000 mg of Mucuna daily in four divided doses. A good dosing schedule is to take 1500 mg in the morning upon waking, again at noon, again at 3 pm, and the final dose of 1500 mg in the evening around 6 pm. In addition to Mucuna pruriens, it’s also important to take at least 25 mg of vitamin B6, 150-350 mg of magnesium, and 15-30 mg of zinc (take with a 2 mg copper supplement) in order to ensure that the L-dopa in the Mucuna bean can actually get converted to dopamine. Without these nutrients, the body is unable to make the conversion, and the Mucuna pruriens may not be as effective. Combine this protocol with Lugol’s iodine 2% at a dose of 1 drop daily for 7 days, increasing by 1 drop weekly up to a total of 20 drops per day (50 mg).
 Click here to buy Mucuna Pruriens.
Click here to buy Mucuna Pruriens.
I
Lugol’s Iodine, 2%
As I’ve already mentioned above, iodine supplementation is important for anyone with a reproductive or endocrine disorder including chronic pain conditions (which always involve imbalances in the endocrine system and often also the reproductive hormones), regardless of gender. Lugol’s iodine solution combines molecular iodine with potassium iodide; while molecular iodine feeds the thyroid gland, and potassium iodide feeds the reproductive organs. Iodoral is another brand of iodine supplement that combines potassium iodide with molecular iodine, but it is quite a bit more expensive such that most people choose to work with Lugol’s.We’ve discussed the idea that iodine deficiency plays a role in chronic pain already in our talk about histamine. Bromide and fluoride toxicity play a role in the drama of iodine deficiency as a body that’s deficient in iodine is vulnerable to the toxic halides bromide and fluoride as well as organophosphates. Most people know that the GMO foods that are grown en masse in the developed world can only be maintained by spraying these crops using either bromide-containing insecticides or organophosphate-containing insecticides. Both bromide and organophosphate-insecticides work through their toxic effects on an insect’s nervous system. The human nervous system functions similarly to that of an insect which is why these substances produce such toxic effects in humans. Of course, a toxin that builds up in the body, like bromide or organophosphate, that impacts the nervous system can definitely produce nervous system dysfunction including chronic pain conditions. Regular, ongoing, high-dose Lugol’s iodine supplementation can protect the body from bromide exposure, in particular which in turn, can reduce chronic pain.
There are a few different reasons why iodine supplementation is essential for both women and men with hyperprolactinemia.
As many readers will know, iodine deficiency interferes with thyroid function. This is especially relevant to this discussion of hyperprolactinemia, since the thyroid and the reproductive organs share such a close relationship, and indeed, thyroid hormones and prolactin are also very closely related in terms of how they interact. The pathway for both thyroid hormone and prolactin production starts in the same place in the brain: the hypothalamus. First, the hypothalamus secretes thyrotropin-releasing hormone (TRH) in response to decreased levels of T3 and T4 thyroid hormones detected in the blood. TRH can then be converted to both/either thyroid-stimulating hormone (TSH) or prolactin. From here, TSH stimulates the release of T3 and T4.

Click here to buy The AlivenHealthy Iodine Bible.
The “ingredients” in T3, the active form of thyroid hormone, is tyrosine (an amino acid) and 3 atoms of molecular iodine (thus the designation ”3” in T3). The “ingredients” in T4, the inactive form of thyroid hormone is tyrosine and 4 atoms of molecular iodine (thus the designation “4” in T4). If you are deficient in iodine, you can’t produce thyroid hormone. If you are deficient in tyrosine, you also can’t produce thyroid hormone. Note that in GMO foods like wheat, corn, and soy, tyrosine as an amino acid is no longer produced by the plant (among other vital nutrients) creating an opportunity for people to also become deficient in tyrosine. Indeed, tyrosine is also the precursor for L-dopa. L-dopa, in turn, is the precursor for dopamine production. Without adequate amounts of tyrosine (or L-dopa supplements like Mucuna pruriens), people can’t produce thyroid hormone OR dopamine (or any of the related neurohormones like noradrenaline and adrenaline to keep the autonomic nervous system balanced).But this is an important transitional point. If a person is deficient in iodine, their body won’t be able to produce T3 and T4 at the urging of TSH in the appropriate way. So, T3 and T4 levels will remain low, even if TSH levels increase. Note that both TSH and prolactin lower dopamine levels, and the synthesis of both of these hormones (TSH and prolactin) is ultimately stimulated by the same physiological status (low levels of T3 and T4). So, as a person’s body produces more TRH, and thus more TSH and (possibly) more prolactin, dopamine levels in their brain will also go down.
In this way, a person’s thyroid health directly affects their prolactin levels. Since hyperprolactinemia is commonly associated with the presence of a prolactinoma (a pituitary gland tumor), which is also likely to be a result of iodine deficiency, it didn’t surprise me to find that iodine deficiency plays a major role in the development of this particular problem of hormone imbalance. Indeed, after women go through pregnancy, they are often low on iodine because the growing fetus needs a lot of iodine in order to produce a healthy nervous system.
Lugol’s iodine solution 2% should be taken at a dose of 20 drops per day (this is a 50 mg dose), ideally in the morning or at least before 2 pm, but if you have chronic pain or any inkling of thyroid disease, start with a low dose of 1 drop daily with the supportive nutrients and increase this dose slowly. It can be rubbed into the skin or taken internally by mixing the drops with a glass of fresh, purified water. If your thyroid gland is functioning normally as far you know, start with 1 drop of solution per day, and work your way up to the 20 drops per day at a pace that feels right to you. If you have a diagnosed thyroid disease, start by taking the supportive nutrients for iodine for 2 weeks to 2 months before you begin to dose yourself with iodine. Many people experience the symptoms of a bromine detox, which we talk about in more depth here. If you experience these symptoms, stay at the dose you’re taking until these symptoms pass, and then continue increasing your dosage up to 20 drops per day of Lugol’s iodine 2%.
Be sure to also take the essential supportive nutrients I’ve listed below with your Lugol’s iodine solution. This is essential. Your body may not be able to use the iodine at all if you don’t ake the supportive nutrients. Start these supplements 2 weeks before beginning to take the iodine supplements if you have a thyroid disorder, and then continue to take them even after you’ve begun taking the iodine. Be sure to lower your thyroid medications as your thyroid begins working properly. If you wish, you can switch from thyroid prescription medications to desiccated thyroid supplement to treat hypothyroidism naturally:
- Vitamin C - 3000 mg/day
- Selenium - 200-400 mcg/day
- Magnesium - 150-350 mg/day
- Vitamin B2 / Riboflavin - 200-400 mg/day
- Vitamin B3 / Niacin - 500-1000 mg/day
- Zinc + Copper - 15 mg + 2 mg/day
- Vitamin K2 / MK-7 - 200-400 mcg/day
- Sea Water Supplement - Take 1 tsp with every 8 ounce glass of water you drink during the day. Click here to learn about the benefits of supplementing with trace minerals via sea water supplementation.
- Unless you live in the artics or southern Argentina / Chile, stop taking a vitamin D supplement if you are currently taking vitamin D.

Click here to buy Lugol's iodine 2%.
Vitamin B Complex
Above, we note that vitamin B2 and B3 are specifically valuable for iodine absorption. Vitamin B6 is essential for conversion of the L-dopa precursor amino acid into dopamine and for dopamine conversion to noradrenaline and adrenaline. Vitamin B12, when deficient in the body, causes dementia and severe nervous system issues that can mimic other serious chronic pain conditions as well as diseases like multiple sclerosis. But all of the B vitamins are essential for nervous system health so we recommend that people with chronic pain take a vitamin B100 complex daily. A vitamin B100 complex contains a higher-than-usual dose of each of the B vitamins, but note that if you have a thyroid disease, you need even higher doses of vitamin B2 (up to 400 mg daily) and vitamin B3 (up to 1000 mg daily).Vitamin B12 is found in animal products so anyone who is vegan or vegetarian is at risk of developing a vitamin B12 deficiency which is a serious thing that causes digestive disturbances, thought and memory disturbances, nervous system disturbances, chronic pain and more. If you have Crohn’s disease, ulcerative colitis, or any number of serious digestive issues, you may not be able to absorb vitamin B12 from food (it is found in animal products). If you are over the age of 50 years, you should be receiving an annual or bi-annual vitamin B12 injection because the digestive system cannot absorb vitamin B12 easily past the age of 50 years. In the recent past, doctors used to give patients over age 50 a vitamin B12 shot every time the patient came in for treatment. This practice was discontinued in favor of allowing patients to develop dementia as a result of vitamin B12 deficiency, a much more profitable outcome for Big Pharma.

Click here to buy The Cancer Cure Catalog 4-volume series.
Vitamin B17 is a well-known cancer cure (at least, outside of the US) with a near-100% cure rate in patients who are given this nutrient before receiving chemotherapy or radiation. Since 50% of hyperprolactinemia patients are diagnosed with their condition due to the presence of a pituitary gland tumor, this nutrient deserves a special mention here. Vitamin B17, which is also known as amygdalin or Laetrile, is able to not only cure, but also prevent, cancer, tumors, autoimmune diseases, and degenerative disease states.The vast majority of foods in the US (and many other countries, too, for that matter) have little to no vitamin B17 content in the diet anymore because the foods have been genetically engineered to contain no seeds (for example watermelon and grapes). Or, alternatively, we, The Public, have been taught to believe that the seeds are a) bad for you, b) might kill you, or c) aren’t of any nutritional value at all, and that you can and maybe should just spit them out because they’re “not fun to eat”. This is unfortunate, since vitamin B17 is one of the main nutrients present in these seeds and vitamin B17 can prevent cancer. While most seeds with an almond-type shape contain some vitamin B17, including almonds themselves, the richest form of vitamin B17 can be found in bitter apricot kernels. For Americans, bitter apricot kernels generally offer the most accessible form of vitamin B17 as well as the energy-producing vitamin B15 (which, like vitamin B17, is not included in a vitamin B100 complex product). Abroad, this nutrient can be found much more freely in supplements as well as in the form of injections given by medical doctors at certain cancer cure clinics.
Vitamin B17 can be taken at a dose of 500-1000 mg/day, or at a dose of 20 apricot kernels taken in 4 divided doses throughout the day (eat only 5 apricot kernels per sitting).
 Click here to buy Bitter Apricot Kernels.
Click here to buy Bitter Apricot Kernels.
As I already talked about above, vitamin B6 must be taken with Mucuna pruriens in order to support the conversion of the L-dopa amino acid to the neurotransmitter dopamine. One important connection here, again, is between prolactin and dopamine; when prolactin increases, dopamine levels decrease, and when dopamine levels go up, prolactin levels go down. So, therefore, one can assume that many natural medicines that support the production and utilization of dopamine would help regulate prolactin levels and help bring them back within a normal range. Vitamin B6 deserves special attention in its role in the production and release of dopamine.
To illustrate the potential efficacy of vitamin B6, one study observed that vitamin B6 administration, without any other medicines, proved to be nearly as effective as the drug cabergoline in the management of hyperprolactinemia. The patients in the study who received vitamin B6 supplements exhibited a 52% reduction in prolactin levels, an 18% reduction in luteinizing hormone levels, and a 31.5% increase in growth-hormone levels. The patients receiving vitamin B6 supplements reported no side effects for the whole duration of the treatment, while the patients receiving cabergoline, in contrast, had headaches and hypotension (low blood pressure).
This particular study gave patients a daily dose of 300 mg of vitamin B6, which is quite high for long-term use, but it still stands to reason that if a hyperprolactinemia patient were to take 25-100 mg of vitamin B6 daily in combination with a medicine like Mucuna pruriens that this may produce the same, if not better, results over the course of time. Most vitamin B100 complex products contain 100 mg of vitamin B6 which is a very respectable dose of this vital nutrient for chronic pain.
Pancreatic Enzymes
Pancreatic enzymes are another core treatment for patients with tumors or cancer of any kind, but they’re also important for chronic pain relief. Though pancreatic enzymes are essential for healthy digestion (and therefore healthy absorption of nutrients from food or supplements), they are also known to be reabsorbed by the intestines into the blood supply, where they then circulate to all of the cells in the body via the blood. Pancreatic enzymes can target cancerous cells to dissolve these cells’ protective covering, thus making the unhealthy cells visible and vulnerable to the immune system. Since 50% of hyperprolactinemia cases are caused by prolactinoma, a pituitary gland tumor, patients with this specific cause of hyperprolactinemia may benefit from the use of pancreatic enzymes. Click here to buy Pancreatic Enzymes.
Click here to buy Pancreatic Enzymes.
Pancreatic enzymes and the non-endogenous enzyme serrapeptase can be used to get rid of fibrotic tissues throughout the body that may cause chronic pain by producing adhesions among other things. Pancreatic enzymes break down living fibrotic tissue while serrapeptase breaks down dead fibrotic tissue. And pancreatic enzyme therapy helps the body absorb the nutrients that help the body heal itself when chronic pain is an issue.
Read more about how pancreatic enzymes work and how they should be taken at this link.
Learn about the specific benefits of enzymes for increasing fertility here.

Click here to buy Serrapeptase.
Vitamin B6 / Pyridoxine
As I already talked about above, vitamin B6 must be taken with Mucuna pruriens in order to support the conversion of the L-dopa amino acid to the neurotransmitter dopamine. One important connection here, again, is between prolactin and dopamine; when prolactin increases, dopamine levels decrease, and when dopamine levels go up, prolactin levels go down. So, therefore, one can assume that many natural medicines that support the production and utilization of dopamine would help regulate prolactin levels and help bring them back within a normal range.To illustrate the potential efficacy of vitamin B6, one study observed that vitamin B6 administration, without any other medicines, proved to be nearly as effective as the drug cabergoline in the management of hyperprolactinemia. The patients in the study who received vitamin B6 supplements exhibited a 52% reduction in prolactin levels, an 18% reduction in luteinizing hormone levels, and a 31.5% increase in growth-hormone levels. The patients receiving vitamin B6 suppleents reported no side effects for the whole duration of the treatment, while the patients receiving cabergoline, in contrast, had headaches and hypotension (low blood pressure).
 NOW Supplements, Vitamin B-6 (Pyridoxine HCl) 100 mg, Cardiovascular Health*, 250 Veg Capsules
NOW Supplements, Vitamin B-6 (Pyridoxine HCl) 100 mg, Cardiovascular Health*, 250 Veg Capsules
Herbal Medicines for Hyperprolactinemia
Ayurvedic Herbal Treatment for Hyperprolactinemia
One recent study done in 2021 observed the complete recovery of a 21-year-old woman with hyperprolactinemia caused by a secretory pituitary microadenoma. The woman was diagnosed with the condition following complaints of menstrual irregularities and disturbances. She was treated using Shamana Nasya for the first 7 days of treatment, and then with Shamana Cikitsa for 3 months after that. 6 months after beginning the study, the woman maintained regular prolactin levels and her pituitary tumor had completely disappeared. A different case report on a 28-year-old woman with hyperprolactinemia and PCOS demonstrated positive results with the use of the Stanaysodhana Gana combined herbal treatment. By the end of the 3 month treatment period, the patient displayed lower serum prolactin levels, and her menstrual cycle had regularized. The woman’s luteinizing hormone and follicle stimulating hormone levels were also within the normal, acceptable range. The medicine known as Stanaysodhana Gana includes these herbs:- Abuta / Laghu Patha / Ponmusutai (Cissampelos pareira)root
- Ginger (Zingiber officinale) rhizome
- Deodar / Himalayan Cedar (Cedrus deodara) bark
- Purple Nutsedge / Nutgrass (Cyperus rotundus) rhizome
- Marsdenia tenacissima root
- Guduchi (Tinospora cordifolia) stem
- Holarrhena antidysenterica seed
- Bitterstick (Swertia chirata) whole plant
- Kutki / Katuka (Picrorhiza kurroa) rhizome
- Indian Sarsaparilla (Hemidesmus indicus) whole plant

Click here to learn more about the DreamLight.app, a guided meditation and brain-entrainment tool.
Bushen Huoxue - Traditional Chinese Herbal Remedy for Hyperprolactinemia
Traditional Chinese Medicine (TCM) is radically different from the Ayurvedic system of medicine in many ways, yet both systems tend to gravitate toward the use of herbal remedies as primary methods of treatment for disease. Bushen Huoxue is one TCM herbal treatment that has been shown to be effective for the treatment of hyperprolactinemia; this remedy includes the following herbs:- Astragalus / Huang Qi root (Astragali radix / Astragalus aaronii)
- Dong Quai root (Angelica sinensis radix)
- Szechuan Lovage / Chuan Xiong rhizome (Lingustici chuanxiong Rhizoma / Lingusticum acuminatum)
- Tu Si Zi seed (Cuscutae semen / Cuscuta chinensis)
- Mulberry Mistletoe / Sang Ji Sheng stem and branch (Taxilli herba / Loranthus acaciae)
- Xu Duan root (Dipsaci radix / Dipsacus acaulis)
Nigerian Herbal Remedy for Hyperprolactinemia
In many African countries, herbalism is considered the frontline treatment options for most health conditions, including hyperprolactinemia, due to its accessibility, affordability, and the belief that the local populations have in the healing powers of plants. In Nigeria, one specific remedy consisting of 5 herbs has come to be one of the most commonly prescribed treatments for hyperprolactinemia. This treatment combines the tinctures of the leaves of the following herbs in equal quantities:- Common Bamboo (Bambusa vulgaris)
- Bitter Gourd / Bitter Melon (Momordica charantia)
- Poison Devil’s Pepper (Rauwolfia vomitoria)
- Cape Fig (Ficus sur)
- Gung / Glorybowers (Clerodendrum capitatum)
Other Herbal Medicines for Hyperprolactinemia
There are actually many, many herbs that have been proven to lower prolactin levels or otherwise help support recovery for hyperprolactinemia patients. The list would be too long to include here, so we’ve decided to include a brief list of some other studied herbal treatments for this condition. See the resources for studies with more details on how these herbs work and how they should be taken for hyperprolactinemia.- Sage (Salvia officinalis)
- Marjoram (Origanum majorana)
- Celery Seed (Apium graveolens)
- Peony (Paeonia spp.)
- NOTE: Peony combines especially well with licorice root for the treatment of hyperprolactinemia.
- Licorice Root (Glycyrrhiza glabra)
Resources:
 The pituitary gland is located in the brain, and regulates various reproductive hormones.
The pituitary gland is located in the brain, and regulates various reproductive hormones.