Spotlight on the Parathyroid Glands and Reproduction
The four parathyroid glands are usually located in the neck next to the thyroid gland, though in some people, the parathyroid glands are located in a slightly different region of the neck or even in the chest. That's okay. The location of the parathyroid glands doesn't seem to matter. But these little glands don't get a lot of attention unless they're seriously malfunctioning, which is unfortunate because the parathyroids actually impact all systems of the body and if we put a spotlight on the parathyroid glands, some readers may be able to easily see how these glands are ailing to the detriment of their whole-body health.What do the parathyroid glands do?
The parathyroid glands function to regulate calcium and phosphate levels in the blood. Though calcium and phosphate in the bones and teeth work together as equal partners and “ionic soul mates”, in the blood, calcium and phosphate have a different relationship. If calcium and phosphate are in a true-love kind of marital bond in the bones, they are in a turbulent, on-the-verge-of-divorce kind of inverse relationship in the bloodstream. In the blood, as calcium levels go higher, phosphate levels go lower. The parathyroid gland manages this rocky relationship between calcium and phosphate in the blood (not in the bones) in part through its effect on vitamin D and estrogen levels.The Parathyroid Glands and Vitamin D
The parathyroid glands increase the activity of the enzyme that produces the activated form of vitamin D in the body. Vitamin D is naturally produced in the skin in an inactive form when our bodies are exposed to sunlight (without sunscreen). Activation of this inactive form of vitamin D from the skin happens in the liver and in the kidneys. The active form of vitamin D then increases the amount of calcium that's absorbed in the gut and it also prevents calcium from being flushed out by the kidneys.Vitamin D2 and vitamin D3 are active forms of vitamin D. Taking vitamin D2 or vitamin D3 supplements by themselves without vitamin K2 is dangerous because of the effect that these active forms of vitamin D have on blood calcium levels in the blood vessels and other soft tissues. Taking vitamin D in these active forms (vitamin D2 and vitamin D3) can throw off the balance of a system that is finely tuned in people who are already healthy and getting regular sun exposure. The abnormally high activated vitamin D that happens through vitamin D2 or vitamin D3 supplementation can lead to abnormally high calcium levels in the blood, which in turn, can lead to a build up of calcium in soft tissues such as the blood vessels (e.g. arteriosclerosis or atherosclerosis) or in the organs (such as the pineal gland as just one of an infinite number of possibilities).
High Levels of Vitamin D / Dangers of Vitamin D Supplementation in Regard to Blood Calcium Levels
But that's not the only havoc that's wreaked by high levels of activated vitamin D on the body. When average people think of calcium as a nutrient, they mostly think of healthy bones and teeth. According to all those Got Milk ads and Dairy Industry marketing propaganda, more calcium is better, right? Actually, as you'd expect, the health effects of calcium levels in the body aren't as straightforward as dairy farmers might want for us to believe.It isn't common knowledge that calcium works in the body as an electrical ion with a double positive charge. That positive charge makes calcium ions pretty sexy to negatively charged electrolytes like iodine, for example, which means that calcium can pair up with iodine if the two happen to be present in the blood supply in high concentrations at the same time, which is bad news for the thyroid gland and for the reproductive organs. In other words, don't take calcium supplements and iodine supplements at the same time. In fact, skip the calcium supplements altogether. And note that vitamin D supplements hijack your attempt to feed your thyroid and reproductive organs the molecular iodine and potassium iodide that they so desperately need by increasing calcium levels in the bloodstream. While your doctor might be prescribing vitamin D in supplement form or even as injections to help your body produce more testosterone, for example, on the basis that vitamin D is rather like a hormone precursor, these supplements might, through a different biological pathway, cause calcium to be present in the blood in higher than normal quantities that end up captivating the interest of iodine in a love affair that ends with the accidental excretion of too much iodine from the body.

The AlivenHealthy Iodine Bible - Everything you need to know to get started taking iodine and more!
Calcium makes the tightest, healthiest relationships with phosphate ions, which are also negatively charged and these two ions (calcium and phosphate), when they find each other in the right context, settle down in the bones and teeth and take up habitation there as some of the most solid and enduring electrolytic-ionic relationships in the body. Hydroxyapatite is a good example of a calcium-phosphate marriage in the teeth that forms some of the hardest, toughest material in the body (enamel) while maintaining at the same time, a magnetic behavior of being able to breakdown and then remodel and rebuild itself under changing conditions. It would make sense if you were to wonder, is it possible to remineralize teeth? The answer is yes and you can read more about how to remineralize teeth here.
Both calcium and phosphate as separate ionic entities are both pretty attractive, funny, and sexy ions to other ions in the body. In today's world, calcium and phosphate would both probably be social media influencers because of their social charisma, wit, and intellect. They make the perfect couple, but they have to find each other like all soul mates. So a given calcium ion or phosphate ion may spend quite a bit of time and energy dating other ions before they finally find each other and settle down. And some of the relationships with these other ions are pretty hot, I tell you, but not all of them are healthy.
Phosphate ions are incredibly promiscuous in their adenosine triphosphate (ATP) - adenosine diphosphate (ADP) forms, which could be likened (in this little metaphor I'm creating) to a molecular orgy of sorts that releases all kinds of energy on the cellular level. Phosphate in this context is not only healthy, but essential, though you wouldn't know it from my metaphor. Maybe I should expand my metaphor a bit and, instead of implying that phosphate is doing some kind of sexually illicit thing in this ATP-ADP cycle, I should say that phosphate is doing some kind of important and really engaging work that keeps the rest of the body running. Maybe phosphate works in renewable energy promoting the use of solar power or something like that. She's passionate about her work and she talks to and works with a lot of biological systems.
Calcium, on the other hand, often plays hard-to-get with other positively charged ions like sodium that are totally wrong for calcium. Calcium might be rather like a man who has trouble expressing himself in his intimate relationships (that is, until he eventually meets directly with phosphate, that is). Nonetheless positively charged calcium and positively charged sodium ions cross cellular membranes, like star-crossed lovers passing each other the stairs, using a special membrane transport system that is fueled, ironically, by the energy generated by phosphate orgies (the ATP-ADP cycle). Obviously two positively charged ions like calcium and sodium aren't destined to work out though they flirt with each other a lot. And the flirtation is biologically important to our health and well-being, of course.
But calcium and phosphate are never far away from each other in the human body. They're naturally attracted to each other and they're constantly searching for direct contact with each other in different biological contexts.
In the nervous system neurons often need to manage calcium levels in the cell after an action potential is initiated and the cell becomes strongly polarized and then depolarized. So proper calcium levels in cells play a vital role in our nervous system health and in the recovery of neurons after an action potential is initiated. Excitotoxic insults to the nervous system require healthy calcium membrane transporters to be intact (think of the membrane transporters like a subway system) and functioning well to prevent damage to the nervous system. For example, if neurotransmitters like glutamate (due to consumption of monosodium glutamate, for example) become too high and the calcium membrane transporters are too low, too much calcium might linger in the neurons for too long, causing damage to the neurons (like a cheap date that stays too long after a party ends because the subway has closed down). Too much glutamate in the neurons causes a huge influx of calcium ions (to said party via the subway) that then activates enzymes inside the cell that damage cellular structures, including DNA (like a riot or even just a party with too many inconsiderate "calcium" guests).
In summary, calcium levels play this important role in nervous system health. Calcium ions thus, also impact the health of any structure in the body that depends on nervous system input (every tissue and every organ). In particular, the on-again-off-again relationship between calcium and sodium as well as the intense true-love type of relationship between calcium and phosphate can impact all of the following in the human body:
- Neurotransmitter and neurohormone release
- Activity of photoreceptor cells in the eyes and in the skin
- Circadian rhythm abnormalities that may be caused by calcium imbalances or calcium membrane transport malfunction play a big role in an array of different disease states, including noteworthy examples such autism and autism spectrum disorder.
- Cardiac muscle relaxation
- Maintenance of calcium levels in the sarcoplasmic reticulum in heart muscle cells
- Maintenance of calcium levels in all other cells in the body
- Maintenance of calcium levels in the mitochondria (the cellular battery)
- Excitation-contraction coupling
- Cardiac arrhythmias
The main takeaway here is the calcium and phosphate levels are inextricably linked inside the body. If your body is exposed to organophosphates (unhealthy organic, carbon-containing forms of phosphate as opposed to healthy inorganic forms of phosphate) or if you take an organophosphate drug (known as bisphosphonates) to improve the look of bone tissues on x-ray or on other tests (while ultimately harming the bone tissues to make them more susceptible to breakage). Or, if you just eat a lot of foods that contain phosphate additives, increasing your phosphate load to unhealthy and unnatural levels in the body (which simultaneously impacts blood calcium levels), you can end up with some pretty serious health problems that might impact just about any part of your body.
Below we talk about vitamin K2, a natural substance that plays a vital role in regulating calcium allocation in the body. Most people are deficient in vitamin K2 which has globally negative health effects that are often overlooked by doctors and health practitioners.
 Click here to subscribe to the Living Database!
Click here to subscribe to the Living Database!
Vitamin K2
Vitamin K2 is a vitamin that is practically unknown in the developed world despite the fact that it plays a vital role in bone remineralization and remodeling. In fact, vitamin K2 is practically unknown in the developed world because it plays a vital role in bone remodeling to prevent and treat osteoporosis naturally as well as atherosclerosis and the natural ability of human teeth to remineralize when people are not deficient in vitamin K2. The Dental and Orthodontic Industries depend on vitamin K2 deficiency to keep patients lined up for treatment at their doorstep, after all. Babies and children who have plenty of vitamin K2 tend to have straight teeth and jaw bones that are big enough to accommodate all of their very healthy teeth which means that breastfeeding women who are properly charged up with plenty of vitamin K2 won't be spending much money on orthodontics. They'll have children with straight, healthy teeth (in contrast to vitamin K2 deficient breastfeeding women or women who feed their children formula that lacks vitamin K2--they're children will likely need all kinds of help from dentists and orthodontists). Adults who have plenty of vitamin K2 are unlikely to develop osteoporosis or atherosclerosis because vitamin K2 makes sure that the calcium absorbed in the gut (a process facilitated by vitamin D) is placed in bones and teeth where it belongs rather than in soft tissues like blood vessels or organs. So vitamin K2 may not be well known in the developed world, but it certainly plays a starring role in diseases and disorders that conventional medicine doctors can't seem to cure.So now that you understand the important role of vitamin K2 in terms of human health, let's dig into the details of how vitamin K2 works with calcium in the body.
Vitamin K2 plays a vital role in calcium balance in the bloodstream. Studies have shown that a low calcium diet can induce hypocalcemia (low calcium levels in the blood) which, in turn, spurs the parathyroid glands to release parathyroid hormone. Hypocalcemia (low calcium levels) causes a cascade of effects that begins with increases in the production of the active form of vitamin D (1,25-dihydroxyvitamin D [1,25(OH)2D]) in the blood while simultaneously decreasing blood levels of the inactive form of vitamin D (25-hydroxyvitamin D 25(OH)D]. These effects essentially boost the intestinal absorption of calcium to restore balanced calcium levels in the bloodstream. At the same time, the absorption of calcium in the kidneys is stimulated as well. So calcium levels can be managed through several different mechanisms of action in the bloodstream, in the gut, and in the kidneys. That’s why it isn’t usually necessary to take a calcium supplement. There are multiple ways through which the body can manage calcium levels and ensure that there’s plenty of it as long as vitamin D and vitamin K2 are present.
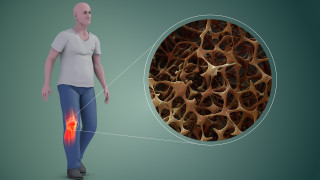
When calcium levels are low in the body and the body is deficient in vitamin K2, the bones release calcium into the blood in small quantities which, over time, can cause the bones to lose a critical amount of bone mass. The bone marrow cavity can be affected through bone calcium losses too. But with vitamin K2 supplementation, a diet low in calcium stimulates calcium absorption by the kidneys to keep blood levels of calcium at normal levels. When the blood calcium levels are kept normal and balanced because the body has plenty of vitamin K2 to address its needs, the parathyroid gland doesn’t release parathyroid hormone in the same quantity or to the same extent which means that bone tissues are not negatively affected in the same way or to the same extent by occasionally low blood calcium levels.
The overall effect of supplementing with vitamin K2 in the body then, is stronger bones and teeth despite daily or hourly changes in blood calcium levels due to diet. In other words, though the balance of calcium in the blood supply might fluctuate, vitamin K2 ensures that that balance does not negatively impact bone density. When there is a deficiency of vitamin K2, the body is compelled to remove calcium from the bones to maintain a balance of calcium in the blood supply.
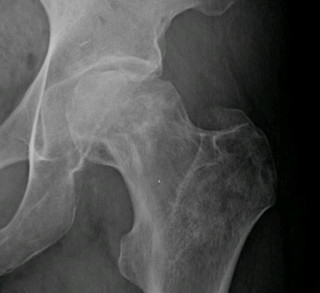
In summary, if you have low bone density, you definitely do not need to take bisphosphonates (or rather, a re-branded form of organophosphates) to improve your bone health. Bisphosphonates do not improve bone health, by the way. Bisphosphonates improve the appearance of bone tissues in x-rays and other bone scanning tests. But though the bone tissues of patients who take bisphosphonates may appear more dense in these tests, the bones are not stronger or healthier. Rather, bisphosphonates create the appearance of health while a large number of patients who take these drugs end up experiencing a specific type of femoral bone fracture years after their bisphosphonate treatment ends. This bone fracture of the thigh bone tends to happen in an unusual location that differs from where patients who have never taken bisphosphonates would experience a thigh bone break. It is this unusual position of the bone fracture and the fact that these bone fractures are so common in those who take bisphosphonates that has alerted to doctors and scientists to the fact that these fractures are actually caused by bone weakening that occurs when patients take bisphosphonates. Read more about the risks of taking bisphosphonate drugs here.
A healthy and natural alternative to bisphosphonates is vitamin K2 /MK-7. Vitamin K2 naturally rebuilds the bone tissue by directing the body to put calcium into the bones and teeth rather than allowing the calcium to circulate in the bloodstream where it can cause serious cardiovascular diseases like atherosclerosis and organ calcification (which is often misdiagnosed as cancer, diabetes, or a wide variety of other diseases). Vitamin K2 is a cure for osteoporosis. It is also a cure for atherosclerosis and other disease processes that involve calcium. Read more about how to use vitamin K2 as a natural cure for osteoporosis and atherosclerosis here.
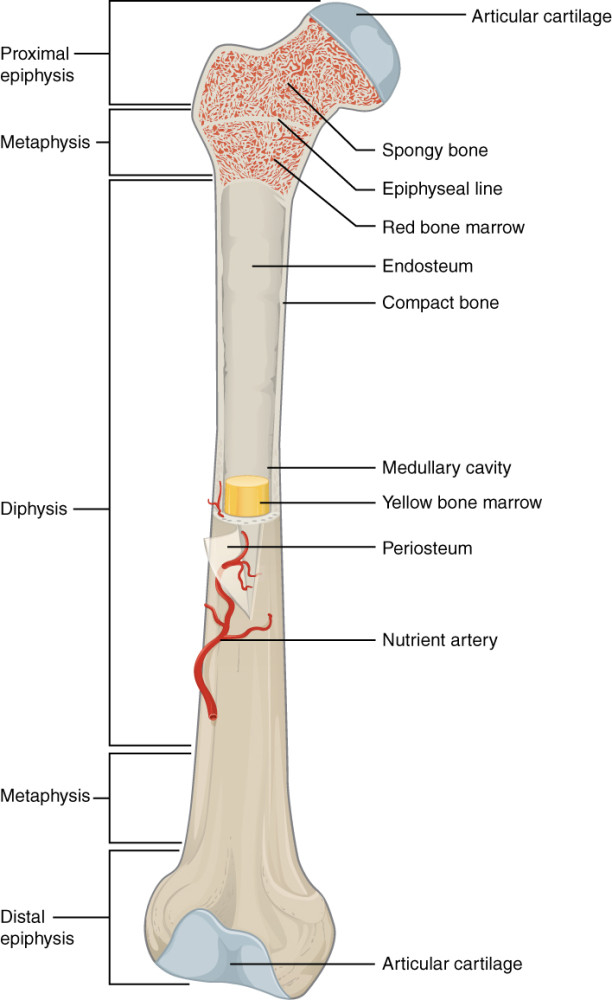
While vitamin K1 is a nutrient that ensures that the soft marrow inside the large bones such as the femur are healthy (it deals with blood and blood-clotting), vitamin K2 works with the health of the outer layer of bone cells to ensure that the hard exterior is strong and healthy. The health of this hard exterior confers health, of course, to the soft interior marrow as well. Obviously the outside of the bone tissue is interwoven with the interior of the bone tissue. So while the body is often able to produce vitamin K1, it’s important that your body has access to vitamin K2 in the form of a supplement if it is not readily available in the diet.
Parathyroid Hormone
The parathyroid glands are like an orchestra conductor that coordinates and regulates blood levels of all of the following:- Calcium
- Phosphate
- Vitamin D
- Estrogens
When levels of any one of the following get too high or too low in the bloodstream, the parathyroid glands respond by releasing more or by releasing less parathyroid hormone. The parathyroid glands are exquisitely sensitive to levels of calcium. When calcium levels are too low, parathyroid hormone secretion is initiated within seconds or minutes. When calcium levels are too high, parathyroid hormone secretion is diminished within seconds or minutes.
In the past, scientists thought that phosphate levels in the blood adjusted dynamically to the balance of calcium in the blood. They thought that calcium levels dictated phosphate levels in the blood such that levels of phosphate were dependent on levels of calcium. But today, there’s a lot of evidence saying that phosphate is actually the substance that triggers changes in parathyroid hormone levels and that calcium levels adjust dynamically to phosphate levels and not the other way around. The influence of phosphate levels on parathyroid hormone is independent of blood levels of calcium or levels of activated forms of vitamin D in the blood.
According to studies on phosphate levels in the blood, low phosphate levels decrease parathyroid hormone secretion and parathyroid hormone levels in the blood. This effect on the parathyroid hormone then impacts calcium levels indirectly. In other words, the blood levels of phosphate don’t interact with or influence blood levels of calcium directly. The parathyroid hormone acts essentially as an intermediary between calcium and phosphate in the blood (not in bone tissues or in the teeth where calcium and phosphate make strong ionic bonds that are broken and then restored over and over again in a process known as bone remodeling). While calcium and phosphate are like lovers or soul mates in bone tissues and in the teeth, they only interact through a marriage counselor (so to speak) in the blood supply. In this metaphor, the parathyroid glands and parathyroid hormone would be the marriage counselor maintaining the relationship between calcium and phosphate in the bloodstream.
Phosphate works directly on the parathyroid gland to decrease parathyroid hormone levels by putting the brakes on gene transcription of the hormone inside parathyroid cells.
But meanwhile, vitamin D3 (activated forms of vitamin D) also directly influence the parathyroid gland. Vitamin D, like phosphate, also has the power to decrease parathyroid hormone levels by slowing gene transcription of parathyroid hormone. So you have two competing factions working to influence the parathyroid gland and the release of parathyroid hormone: serum phosphate levels and serum vitamin D3 levels. Both can tell the parathyroid glands to slow gene transcription of parathyroid hormone to, in turn, make changes in the blood serum levels of calcium.
It’s easy to imagine how taking activated forms of vitamin D could thus lead to serious imbalances in the body through this physiological pathway that I’ve just described. Parathyroid hormone responds primarily to:
- Phosphate levels in the blood
- Activated vitamin D levels in the blood
- Estrogen levels in the blood
In turn, parathyroid hormone then regulates calcium levels in the blood, which impacts kidney health, the health of the heart and circulatory system, nervous system health, reproductive system health, bone health, and blood health.
How to Heal the Parathyroid Glands
We’ve written a lot about the importance of Lugol’s iodine as a nutrient that restores balanced immune function in cancer patients and in patients with autoimmune disease. Indeed, Lugol’s iodine supplementation is used to feed the thyroid gland and the reproductive organs and supplementation with Lugol’s iodine often works as a cure for reproductive organ cancers and thyroid cancer among other things. And when I say, “other things”, I’m seriously abbreviating the extensive list of diseases that respond positively to Lugol’s iodine supplementation. It’s nearly impossible to be healthy in the developed world without taking a Lugol’s iodine 2% supplement at 50 mg per day. And Lugol’s iodine is to the thyroid gland what boron supplements are to the parathyroid gland.That being said, while your thyroid gland needs about 50 mg of Lugol’s iodine (which is a combination of two forms of iodine including molecular iodine and potassium iodide to feed both the reproductive organs and the thyroid), your parathyroid glands needs between 1-6 mg of boron daily in order to be healthy. The profound impact of iodine on human health via the thyroid gland and reproductive organs is equaled by the profound impact of boron on parathyroid organ health.
Boron and Testosterone: Why Boron Raises Testosterone and How Boron Balances Reproductive Hormone Levels
You see, there’s a connection between your thyroid gland and your parathyroid glands besides just their proximity inside the body. High serum calcium levels in the blood can inhibit absorption of iodine in the tissues. So while vitamin D and phosphate are working through the parathyroid glands to regulate the release of parathyroid hormone that in turn regulates levels of calcium in the blood, the body’s ability to absorb iodine is governed to a great extent by these calcium levels. As such, parathyroid function and health is therefore fundamental to thyroid health. You can’t feed the thyroid glands or the reproductive organs iodine if your blood calcium levels are too high due to overproduction of parathyroid hormone (which would lead to hypercalcemia, or high blood calcium levels). Boron is the nutrient that helps your parathyroid glands stay healthy which explains why boron plays such an important role in the production of testosterone. Without it, your reproductive organs won’t be able to gain access to the potassium iodide that they need in order to be healthy.Summary
Calcium and phosphate play many roles in human health. Boron is a nutrient that supports parathyroid hormone health. And the parathyroid glands, in turn, support thyroid gland and reproductive organ health. You can't have a healthy thyroid gland or healthy reproductive organs without the modulating effects of the parathyroids on calcium levels in the body. As we discussed in another, earlier article at this link, Lugol’s iodine and vitamin K2 play a vital role in protecting the thyroid gland, reproductive organs, bone tissues and blood supply from the ravages of organophosphate and bromide-containing insecticide exposure. But without boron to feed the parathyroid gland and manage levels of parathyroid hormone in the body, calcium and phosphate levels can become dysregulated leading to serious health issues including (among other things) reproductive hormone imbalances, fertility problems, and more.
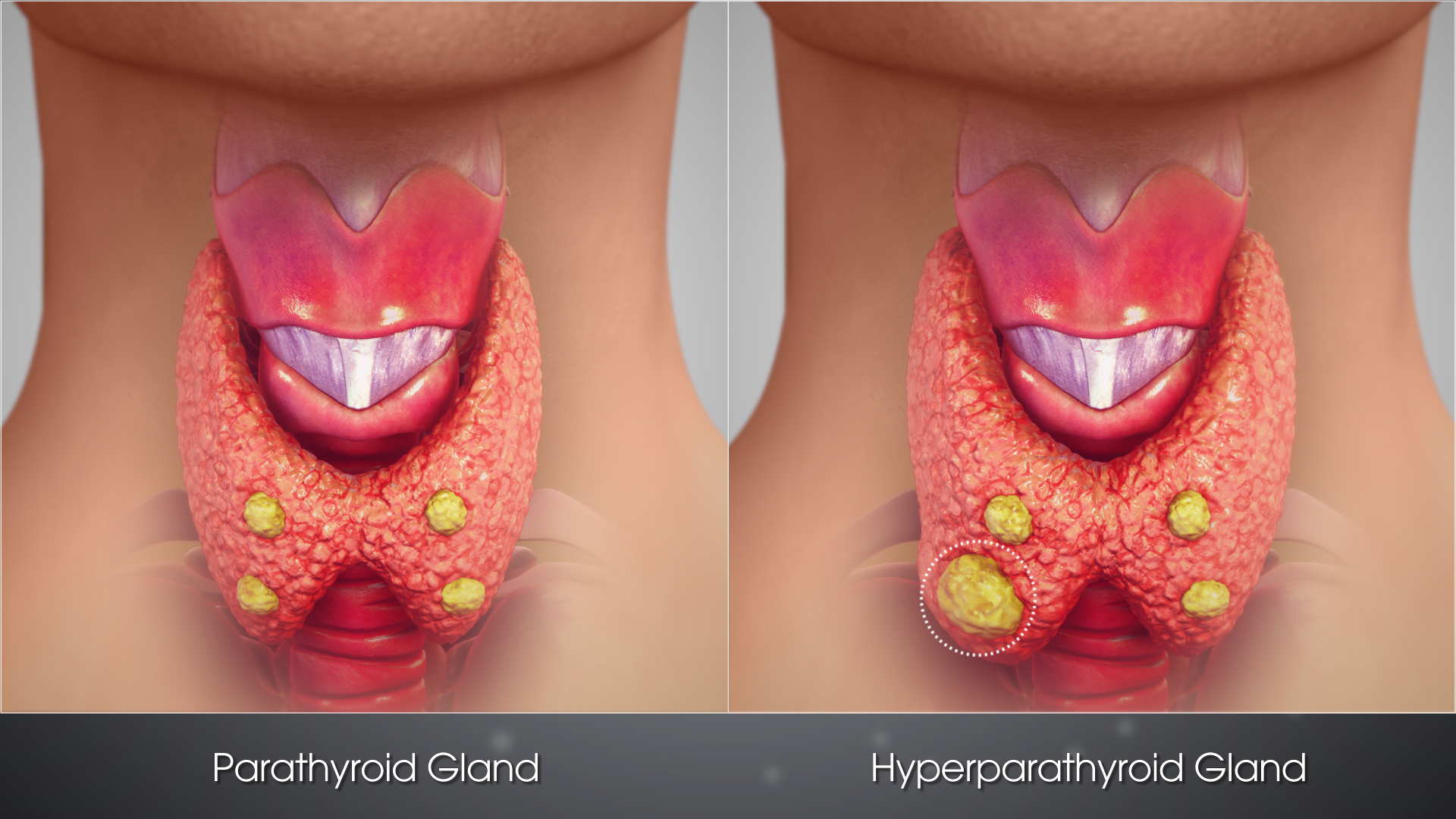 The parathyroid glands are like gatekeepers in terms of thyroid and reproductive organ health. If you don't have healthy parathyroid glands, your thyroid and reproductive organs won't function properly either. And at all ages and stages of life, thyroid and reproductive organ health affects general well-being in a global and powerful way.
The parathyroid glands are like gatekeepers in terms of thyroid and reproductive organ health. If you don't have healthy parathyroid glands, your thyroid and reproductive organs won't function properly either. And at all ages and stages of life, thyroid and reproductive organ health affects general well-being in a global and powerful way. The Origami of Autism: Transforming 2-Dimensional Thinking about ASD into 3-Dimensional Solutions - BUY HERE!
The Origami of Autism: Transforming 2-Dimensional Thinking about ASD into 3-Dimensional Solutions - BUY HERE!