 N-Acetylcysteine (NAC), Acetylcysteine or L-Cysteine as a Cure for Cystic Fibrosis
N-Acetylcysteine (NAC), Acetylcysteine or L-Cysteine as a Cure for Cystic Fibrosis
Thinning mucus secretions is an important part of treating cystic fibrosis and if you have the option to use a substance like N-Acetylcysteine (NAC), L-Cysteine, or Acetylcysteine to thin mucus secretions rather than a prescription or over-the-counter synthetic pharmaceutical. L-Cysteine or NAC are definitely the recommended way to go! L-Cysteine is a natural compound that has a natural and powerful detoxifying effect on the body and the lungs. NAC, in contrast, is a synthetic substance, though it has been extensively studied by scientists. Doctors use NAC to avoid severe liver and kidney damage in patients who have overdosed on acetaminophen because it is such a powerful detoxifier and liver protector. In patients with cystic fibrosis, NAC can be used to thin mucus and also promote general detoxification of the body to reduce the number and severity of recurrent infections that are common in patients with this disease.
In the remainder of this post we talk primarily about NAC, but for many people, it will be easier to get L-Cysteine or Acetylcysteine. Using L-Cysteine or Acetylcysteine may be preferable to using NAC for cystic fibrosis. Just know that when we refer to NAC, we are referring to these three substances, which can be used interchangeably in this context.
NAC has been compared to the drug guaifenesin in terms of its effects on the body. But there’s a difference between NAC and guaifenesin in that NAC is a major detoxifying agent in the body that positively influences physical functioning in terms of mental health and addictions as well as in terms of reproductive health and lung health. NAC is one of the most important natural medicines to keep in your medicine cabinet to treat COVID or influenza because of its strongly positive impact on lung health. It can thin mucus secretions and remove toxins or pathogens that may be making cystic fibrosis worse. And NAC helps remove toxins that may be damaging the lungs to make it easier for patients with this disease to heal.
 L-Cysteine 1000mg | 100 Powder Capsules | Non-GMO, Gluten Free Supplement | by Horbaach
L-Cysteine 1000mg | 100 Powder Capsules | Non-GMO, Gluten Free Supplement | by Horbaach
NAC is safe for use in pregnancy and during lactation and it is safe for use in children. Indeed, studies have examined the use of NAC during pregnancy to prevent intraamiotic infections and inflammation. Women were given NAC for 10 weeks prior to preterm delivery and studies showed that those women had more positive outcomes than the women who had not received NAC during pregnancy. In fact, the pregnant women taking NAC experienced 3 times the number of positive outcomes than women who did not take NAC. This medicine is reported to be feasible, safe, and beneficial to babies and pregnant women.
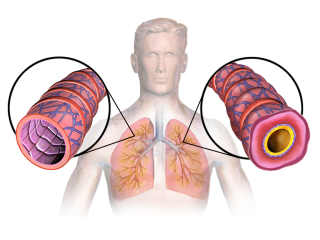
Scientific studies have examined the use of NAC as both an oral supplement and as a compound that can be nebulized into the lungs to reduce viscosity of the mucus. Studies have shown that NAC improves lung capacity and lessens residual air leftover in the lungs. Patients who take NAC have a more even distribution of air in the lungs upon inhalation, and they have an increased flow rate of air as well. Their maximum voluntary ventilation is increased and their respiratory work load is decreased with the use NAC. Cystic fibrosis patients who take NAC are able to exercise more easily and they tend to gain weight and experience better growth.
Below are other effects that cystic fibrosis patients often experience when using NAC:
- Taking 1000 mg daily of NAC for four weeks reduced lung inflammation.
- Lung function is improved with regular use of NAC for 24 weeks.
- The production of normal CFTR protein in animal models who were given high doses of NAC was 12 times higher than in control groups that didn’t receive NAC.
- NAC may positively affect the expression of genes in patients with cystic fibrosis.
Adults should take 1000 mg up to 6 times daily by mouth or nebulize NAC using a product called Mucomyst that may only be available in prescription form through a doctor (see below if you cannot get this prescription medication from your doctor). Children who are old enough to take pills can take between 600 to 2000 mg of NAC daily by mouth. When NAC or Acetylcysteine is inhaled directly via a nebulizer, benefits depend on having a high enough concentration of the medicine and good bronchial drainage after therapy. Aerosols of NAC (under the brand name Mucomyst) have been developed that are sold as 10% or 20% solutions for cystic fibrosis patients.
If you can’t obtain Mucomyst from your doctor, consider nebulizing with a pure N-Acetyl L-Cysteine product or with L-Glutathione Reduced. Combine the N-Acetyl L-Cysteine or L-Glutathione Reduced with nebulizing saline in a nebulizer. This YouTube video shows patients how to combine L-Glutathione with nebulizing saline in a nebulizer to achieve the same effects as Mucomyst, but without a prescription. You will need to add sodium bicarbonate to the L-Glutathione mixture in order to emulsify the ingredients properly.
 Modudose Saline Solution for Inhalation - 100/box(5257-5mL Unit Dose)
Modudose Saline Solution for Inhalation - 100/box(5257-5mL Unit Dose)


Resources:
 BULKSUPPLEMENTS.COM Glutathione Reduced Powder (Reduced Glutathione) - for Antioxidant & Liver Support - Gluten Free, Soy Free - 500mg per Serving (50 Grams - 1.8 oz)
BULKSUPPLEMENTS.COM Glutathione Reduced Powder (Reduced Glutathione) - for Antioxidant & Liver Support - Gluten Free, Soy Free - 500mg per Serving (50 Grams - 1.8 oz)