 Seizures Misdiagnosed as Epilepsy and More…
Seizures Misdiagnosed as Epilepsy and More…
Though American and European doctors are not trained to recognize it, there is an extremely common parasite infection that Indian, Asian, and Latin American doctors readily recognize as the cause of up to 30% of so-called epileptic seizures in children and adults. This parasite infection is the most common helminthic neurological infection worldwide, but many patients with this infection never receive the proper diagnosis which can cause them and their family members a lot of grief, high medical bills, and other tragic losses as a result.
Epilepsy is a common neurological disorder that affects both children and adults of all ages. The designation “epilepsy” means essentially the same thing as “seizure disorder”. A person with epilepsy is basically a person who has experienced a seizure of unknown origin.
People with epilepsy may experience a wide range of different types of seizures. The seizures are unprovoked in epilepsy. In other words, there is no identifiable trigger that causes the seizures in those who are diagnosed with epilepsy. This is important because the lack of a known cause means that doctors can offer no cure. If there is no identifiable cure, treatments to cover up the symptoms of epilepsy are the only option for patients, particularly in the developed world (the U.S. and Europe) where doctors are not trained to look for a different epilepsy diagnosis.
In contrast, in India, doctors know that about 30% of patients who have seizures that would be diagnosed as epilepsy in the U.S. are caused by neurocysticercosis, or parasite infection that affects brain tissue. Certain inspired doctors in the U.S. and Europe have openly admitted that neurocysticercosis is probably as common in developed countries as it is in Asia, Latin America, and everywhere else in the world except Antarctica, but many of them claim that their ability to recognize this parasite infection is an unfortunate consequence of immigration, which is a tragic assessment for people who are a part of the intelligentsia in the developed world. It doesn’t take a genius to put pet ownership into the parasite-infection equation, particularly since we deworm our pets to protect them against the very infection that can cause the symptoms of epilepsy though humans themselves often cannot get these medications to prevent this type of infections after we clean the litter or regularly pick up doggie doos during walks in the city.
Seizures can be caused by reversible medical conditions such as low blood sugar, high fever, or alcohol withdrawal. When a seizure is caused by a reversible medical condition, the patient should not receive a diagnosis of “epilepsy”. Doctors in the U.S. and Europe often recognize blood sugar level issues, high fever, or seizures caused by alcohol withdrawal. These should not be diagnosed as epileptic seizures.
Some patients with epilepsy develop the disease as a result of brain injury that is not caused by neurocysticercosis. In this case, patients may not benefit from anti-parasite treatments. But in some cases, patients with brain injury may still benefit from the treatment. Infection with the Taenia parasite is extremely common, though the infection rarely produces symptoms of any kind. Many people who have epilepsy experience more than one type of seizure and they may have other neurological problems and symptoms which makes sense given the nature of the tapeworm infection in the brain. Indeed, tapeworm infection is pleomorphic, which means that it can “change shape” quickly, which is confusing to doctors. A common misdiagnosis in patients without seizures who have this type of infection is brain cancer because tapeworm infection can easily “metastasize” with the same appearance and behavior as cancer.
This article covers a reversible medical conditions that is commonly misdiagnosed as epilepsy. That disease is neurocysticercosis. This reversible medical conditions can be treated to cure epilepsy permanently if this is the underlying cause of the seizure condition.

Parasites: Self-Treatment and Prevention - BUY THE eBOOK HERE!!!
Neurocysticercosis as an Epilepsy Misdiagnosis
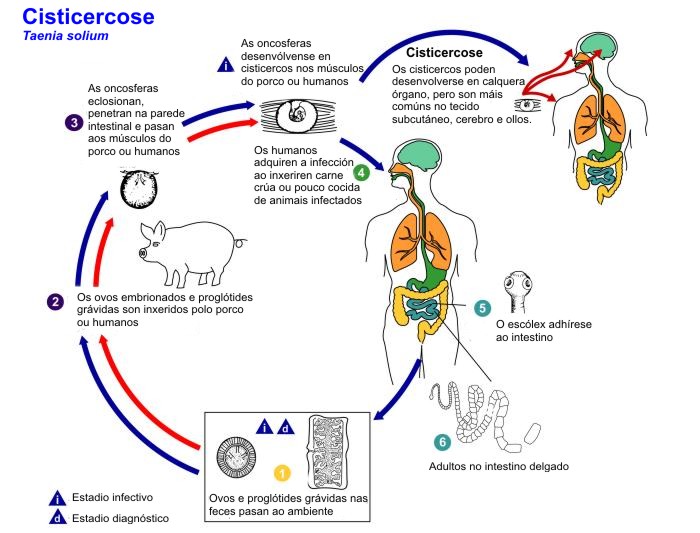
Neurocysticercosis is one of the leading causes of seizures and epilepsy throughout the world. Cysticercosis is a parasitic infection of Taenia solium. It develops when a patient accidentally ingests the eggs from an adult tapeworm. Neurocysticercosis involves infection with Taenia solium that affects the brain tissue.Though infection with Taenia solium used to be a problem that only affected patients in developing countries, this type of infection has been recognized by certain doctors in the United States. For example, in 1983, about 80 patients were admitted to Los Angeles County Hospital with cysticercosis annually, but by 1994, this average had increased by 50% with an average of 120 patients admitted to Los Angeles County Hospital annually. In the southwestern U.S., about 10% of emergency room visits due to seizures were caused by cysticercosis. Those with seizures misdiagnosed as epilepsy in a clinic outside of the emergency room, however, were not included in this study.
Epilepsy Cures and Treatments for Neurocysticercosis Patients Who Have Been Misdiagnosed
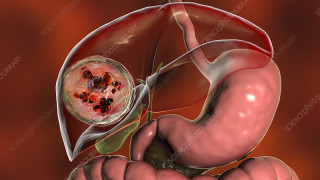
When the eggs of a tapeworm are ingested, they are exposed to hydrochloric acid in the stomach which melts their protective capsule. Once this occurs, the eggs turn into a larval cyst called an “oncosphere”. An oncosphere can easily pass through the gastrointestinal tissue into the bloodstream to eventually find its way to the brain, muscle tissues, and eyes as well as other organs in the body (see Autoimmune Hepatitis for more information about tapeworm larvae in the liver).
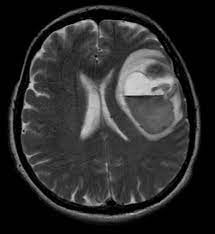
Neurocysticercosis is typically first diagnosed when the patient has their first seizure or a chronic headache. Typically, the cysts that are in a process of degeneration tend to cause the most seizures because the larvae are releasing toxic substances into the brain. Some patients develop an intense inflammatory response while others experience no inflammation. Indeed, some patients experience inflammation in one cyst, but not in adjacent cysts in the brain.
Nonetheless, patients who believe that their seizures have been misdiagnosed as epilepsy should not that cysts that are degenerating often cause the seizures because they are releasing toxins into the brain as they die. Spontaneous cures for epilepsy and other diseases caused by tapeworm infection are not uncommon according to scientific literature in countries where doctors are trained to recognize the disease, but it is also possible to cure the disease using albendazole and praziquantel or chlorine dioxide and DMSO. Treatment should proceed with caution. Chlorine dioxide and DMSO is a treatment that can be used by patients at home, but patients should begin with a very low dosage by following Jim Humble’s MMS starting procedure. Because seizures can be caused by toxin release in the brain that happens as the tapeworm larvae die, it is important to take low doses to prevent the death of too many parasites too quickly for the body to detox.
How Common is Neurocysticercosis in the United States and Other Developed Countries?
On the Indian subcontinent, in Latin America, Africa, and China, neurocysticercosis is a common disorder that affects about 1 out of 1000 people and doctors recognize that patients who have seizures from a seemingly unknown cause may have a tapeworm infection that has passed the blood-brain barrier to lodge in the brain. About 30% of epilepsy cases are caused by neurocysticercosis in these countries, but doctors in the U.S. and Europe have been taught that tapeworm infections are extremely uncommon in the developed world though a large number of people have pets and actively de-worm their pets to prevent tapeworm infection in the pet (not in the humans). The myth that parasites do not exist in “developed” countries has allowed for the development of supposedly new and incurable diseases to proliferate. And patients are given a wide array of new and expensive prescription medications that not only fail to cure epilepsy completely, but that may make the disease worse (particularly if the seizures are caused by neurocysticercosis). Many incurable diseases can be cured through regular parasite cleanses, which were common in the early 1900s. Today, many people who are diagnosed with cancer, autoimmune diseases, and even epilepsy often have parasite infections that can be treated with common drugs like albendazole and praziquantel or chlorine dioxide solution (also known as Miracle Mineral Solution or MMS) and dimethylsulfoxide. As noted above, starting in 1994, at the Los Angeles Hospital in California, neurocysticercosis caused about 10% of the seizures that brought patients to the emergency room.
One case study in the scientific literature involving a 29 year old man who suddenly began having tonic-clonic seizures told a common story that many Americans can relate to. This young man was originally from India. He had moved to the United States 6 years prior and he suddenly had his first episode of tonic-clonic seizures with confusion and loss of consciousness. Doctors in the U.S. diagnosed him with meningioma of the brain and brain surgery was scheduled. But the man didn’t believe the diagnosis and refused the surgery and instead traveled back to India for a second opinion. In India, the doctor diagnosed the man with neurocysticercosis and the patient was given albendazole and steroid medications as part of his comprehensive treatment.
In Europe (particularly Spain and Portugal), some doctors have finally started to notice that epilepsy is often caused by the presence of tapeworm eggs in the brain. These doctors view the problem as an “epidemic” in that the prevalence of tapeworm infections in the brain is similar to that of the Indian subcontinent.
In short, doctors in developing countries believe that they are starting recognize misdiagnosis of epilepsy and seizures because of new technologies that are allowing them to easily look inside the brain though they sometimes speculate that the problem is caused by immigration from poorer areas of the world, but a more likely explanation is the fact that tapeworm eggs can easily be ingested when dog owners or cat owners clean the litter or pick up their animals poop in the park. Indeed, it is possible to catch a tapeworm infection in a strong dust storm carrying the eggs into the body. In Muslim countries, for example, people do not keep household pets due to religious beliefs and they regard pet ownership in developed countries as “dirty”, though they do feed street animals and care for them without inviting them into their homes. The knee-jerk reflex to blame immigration for parasite infection that is likely caused by exposure to pets who have tapeworm infection is uninspired to say the least. Nonetheless, patients with neurocysticercosis who have been misdiagnosed with epilepsy should know that treatment, luckily, is simple if you find a doctor to properly diagnose the disorder. Regular de-worming parasite cleanses should then be undertaken every 6 months after the infection fully clears.
Epilepsy Cured Completely: 30% of Epileptic Seizures Are Caused by Neurocysticercosis
Neurocysticercosis, or tapeworm larvae eggs that have colonized the brain can masquerade as a variety of other diseases that doctors in the United States and other developed countries are not trained to recognize. Misdiagnosis of neurocysticercosis may take any of the following forms:
- Hydatid cyst
- Brain cancer or metastasis (because the eggs may move to other locations in the body that is similar to the way cancer metastasizes)
- Meningioma
- Tuberculoma
- Brain abscess
- Meningitis
- Hydrocephaly
- Autoimmune neurological diseases such as autism
- Schizophrenia or psychosis
- Sleep apnea
- Anxiety
- Migraine or severe headaches
- Intellectual deterioration
Epilepsy Misdiagnosed as Autism
There is a correlation between epilepsy and autism. Indeed, studies have shown that in populations of patients with autism, up to 1 in 3 will develop epilepsy during childhood or adolescence. In India, doctors have noted a correlation between autism and neurocysticercosis in some instances as well. Children, after all, may be disproportionately affected by tapeworm eggs in feces in the soil or that animals may be carrying (some cats and many dogs, for example, may roll around in the litter box or in feces on purpose, which means that they can be carrying the eggs in their fur).
In some children who have been diagnosed with autism (or epilepsy) it is possible that a neurocysticercosis infection is the underlying problem. Extraparenchymal neurocysticercosis can, in fact, cause an autoimmune reaction in the brain that scientists have observed in cerebrospinal fluid. A number of children have had success following Kerri Rivera’s protocol for how to cure autism and it is possible that this technique for using chlorine dioxide and DMSO is able to cure autism by getting rid of parasites though Rivera acknowledges that there may be more than one pathogen infecting the body when a child develops autism. Nonetheless, if you’re looking for a cure for epilepsy in children, Kerri Rivera’s protocol for autism is detailed and provides extensive dosing instructions along with numerous stories of success in treating another major brain disorder: autism.
Epilepsy Misdiagnosed as ADHD or Conduct Disorder
ADHD is associated with pinworms, another type of parasite infection, but as it turns out, Attention Deficit Hyperactivity Disorder also has associations to neurocysticercosis and epilepsy as well. One study linked focal seizures to attention deficit. Scientists noted that attention deficit and hyperactivity as well as conduct disorder could sometimes be explained by the presence of tapeworm larvae infection in brain tissue.
Epilepsy Misdiagnosed as Schizophrenia
Neurocysticercosis can include symptoms of schizophrenia or psychosis. So there is a well-documented correlation between neurocysticercosis and schizophrenia as well as a correlation between neurocysticercosis and epilepsy. As such, a person who has been diagnosed with either or both of these diseases may want to consider diagnosis and/or treatment for neurocysticercosis as a possible cure for schizophrenia as well as a cure for epilepsy.Epilepsy Misdiagnosed as Migraine
Epilepsy and migraine headaches have certain features in common. For example, patients with epilepsy and patients with migraines may both experience visual phenomena. Doctors may tend to misdiagnose epilepsy as migraine or vice versa.One case study noted two patients who had epilepsy misdiagnosed as migraine for two years before receiving the correct diagnosis. Both patients experienced frequent visual seizures that were followed by migraine-like headaches. The seizures involved colorful, circular visual hallucinations that lasted about 1 minute followed by a severe headache that was accompanied by nausea, light sensitivity, and sound sensitivity.
The diagnostic overlap between migraines and epilepsy has led some scientists to consider using the term “migralepsy”. But this new diagnostic label does absolutely nothing for patients who wish to cure epilepsy or migraine headaches. Rather than examining the close relationship between migraines and epilepsy, we need to look at neurocysticercosis as an underlying cause of both of these diseases. A patient with neurocysticercosis can permanently cure migraines as well as epilepsy, after all if they are given the proper medications.
Epilepsy misdiagnosed as migraines is less common in areas of the world where doctors are trained to diagnose tapeworm infection. Visual phenomena, migraines, and epileptic seizures stop after proper treatment is administered for neurocysticercosis if this is the underlying cause of the disease.
Vitamin B6 Deficiency and Misdiagnosis of Epilepsy in Infants
Some children are born with inborn traits that cause a deficiency of vitamin B6 that results in epileptic seizures in infancy. The technical name for this disorder is "PNPO-dependent neonatal epileptic encephalopathy" or NEE. This is a type of epilepsy that doesn't respond to drug treatment, but the good news is that it does respond to treatment with vitamin B6 (B6 vitamers and/or pyridoxine). Phosphatase deficiency or hypohosphatasia disorder may responds to vitamin B6 treatment.Cures for Epilepsy Misdiagnosed as Neurocysticercosis
Albendazole and Praziquantel
Albendazole and Praziquantel are antiparasitic medications that are typically used to treat neurocysticercosis. In some cases, taking these or other antiparasitic drugs can cause brain inflammation and increased intracranial pressure, an increase in seizures as the larvae are expelled from the brain tissue, and sometimes, death. Side effects, however, are usually mild and include nausea, seizures, headache, and cerebral edema. Deaths associated with antiparasitic treatment is rare at only 1-4%. Most of the patients who die from antiparasitic treatment have hydrocephalus and more than 20 cysts in their brain.Albendazole Dosage: 15 mg / kg of body weight divided into 2 doses, taken with meals Praziquantel Dosage: 20 mg / kg of body weight
Ivermectin to Cure Neurocysticercosis
There are several scientifically documented cases wherein neurocysticercosis was cured using ivermectin. Though albendazole by itself or albendazole and prazinquantel together are the recommended course of treatment for neurocysticercosis, ivermectin has also been successfully used to treat this disease. Though doctors may be reluctant to admit to a parasite infection, patients can treat themselves for neurocysticercosis using ivermectin, though they should be mindful of following dosage requirements if they choose to use a veterinary medication instead of ivermectin prescribed by a doctor. Initially, treatment with ivermectin may lead to an increase in seizures as well as a risk of brain inflammation.Ivermectin dosage: 10 mg once daily for 30 days
NOTE: Praziquantel can be combined with Ivermectin if albendazole is not available as a neurocysticercosis treatment.
Chlorine Dioxide and Dimethylsulfoxide for Neurocysticercosis
Chlorine Dioxide (CDS), also known as Miracle Mineral Solution (MMS), is a Reactive Oxygen Species Medicine that can be mixed with Dimethylsulfoxide (DMSO), an extremely non-toxic, FDA approved medication, to treat neurocysticercosis. Chlorine Dioxide is a water-purification agent that is present in trace amounts in water throughout the world to kill a broad spectrum of viruses and bacteria, but it can be used in slightly higher doses to treat a broad spectrum of diseases and disorders that have otherwise been deemed incurable.Though Chlorine Dioxide can easily get past the blood brain barrier to kill pathogens by releasing oxygen that causes the pathogens to explode (leaving behind nothing but common table salt or sodium chloride), DMSO increases the power of this medicine. DMSO specifically heals nerves and brain tissues and it can have miraculous effects on nervous system problems. Chlorine Dioxide can be administered in minute doses initally, gradually increasing the dose over time to prevent strong detox reactions such as seizures or brain inflammation when the parasites begin to die.

Resources:
Ghatge, M.S., Al Mughram, M., Omar, A. M., Safo, M. K. (2021). Inborn errors in the vitamin B6 salvage enzymes associated with neonatal epileptic encephalopathy and other pathologies. Retrieved March 23, 2022 from https://pubmed.ncbi.nlm.nih.gov/33421502/
 The Origami of Autism: Transforming 2-Dimensional Thinking about ASD into 3-Dimensional Solutions - BUY HERE!
The Origami of Autism: Transforming 2-Dimensional Thinking about ASD into 3-Dimensional Solutions - BUY HERE! Click here to sign up for the CDS Protocols App!
Click here to sign up for the CDS Protocols App!