How to Heal a Fistula Naturally
There are many different types of fistulas that can occur for many different reasons in different areas of the body. A fistula is an abnormal tube-like passage between a hollow / tubular organ and the surface of the body or between two hollow / tubular organs. In the developed world, fistulas of the vaginal, rectum (perianal fistula and anal fistula), abdominal fistulas, gum fistulas, and obstetric fistulas, are typically caused by the presence of Inflammatory Bowel Disease such as Crohn’s Disease or Ulcerative Colitis and/or infectious pathogens that are living somewhere in the body. In some cases, however, fistulas are caused by radiation therapy. Indeed, a fistula may develop years after tissues have been assaulted by surgery, radiation, or infection but if you have a fistula that suddenly developed without warning, it is likely due to an infection. And if you have an inflammatory bowel disease, the goal would be to cure Crohn’s disease or ulcerative colitis while also working to heal a fistula naturally.Learn more about Reactive Oxygen Species Medicines that can be used to cure ulcerative colitis, Crohn’s disease, or other types of inflammatory bowel disease here. Then continue reading about additional treatment options to heal a vaginal fistula, gum fistula and oral fistulas, anal fistula, or even abdominal fistula. Reactive Oxygen Species Medicines and Dimethylsulfoxide treatments can be used to heal fistula openings naturally. Vaginal fistulas (including both rectovaginal and vesicovaginal) as well as gum fistulas or fistulas that develop in the mouth may also benefit from the use of Methylene Blue and Red Light Therapy (also known as Photodynamic Therapy). Reactive Oxygen Species Medicines and DMSO, however should NEVER be used with Methylene Blue and Red Light Therapy. These two types of treatment will cancel each other out and render the other useless!
Click here to learn more and subscribe to the Living Database now.
Can a fistula heal itself?
In our view, our bodies always heal themselves. Sometimes, patients need assistance and tools to cure disease and then, the biggest challenge for patients today is simply finding information about legitimate tools that are available for them to use at home. Essentially, if you have a super-broad-spectrum antibiotic tool like Reactive Oxygen Species Medicine that you can use to heal a fistula naturally using the exact same singlet oxygen species that are released by white blood cells in the human body, then you will also likely find that the underlying disease process, which likely includes an inflammatory bowel disease or some other type of infection process, also clears up. In some cases, a fistula may be caused by exposure to radiation. In that case, the cells in the area around the fistula are very low on energy. Energizing the cells is essential in these situations, but patients must proceed with caution, of course and listen carefully to their bodies while using at home treatments like Photodynamic Therapy. Also, DMSO is a substance that is known to protect the body from radiation and it can be used in measured doses to help irradiated cells detoxify and heal.Patients may find that exposing fistulas that have developed due to radiation exposure to Red Light Therapy may help the cells regain energy so that they can heal. Again, it is possible to take doses of Methylene Blue by mouth (at a 1 mg/kg body weight dose). The Methylene Blue then goes into the blood stream where it interacts with the Red Light that is shone at the fistula. Methylene Blue donates electrons to mitochondria in cells that may be lacking electrons (and thus electricity / energy) that they need to heal themselves. Again, do not use Methylene Blue with DMSO or with Reactive Oxygen Species Medicines. You can, however, use Red Light Therapy while treating the body with Reactive Oxygen Species Medicines and DMSO.

Click here to schedule a health coaching session with us.
Photodynamic Therapy at Home to Heal Fistula Openings
If you have a fistula in your mouth, in your perianal region, or in your vagina and you aren’t taking anti-depressant medications or other pharmaceuticals, you can take Pharmaceutical Grade Methylene Blue by mouth at a dose of 1 mg/kg of your body weight. Divide this amount in half so that you can take the divided half-doses two times per day. Within 15-30 minutes of taking the Methylene Blue, shine a therapeutic red/infrared light at the area with the fistula. Shine the red light at the fistula for 5-15 minutes per session.Again, do not take Reactive Oxygen Species Medicines while taking Methylene Blue because these two medicines can cancel each other out. Also, DMSO increases cellular penetration of medicines like Methylene Blue so it should not be used with Methylene Blue.
Get a special red light that can be inserted into the vagina to treat vaginal fistulas that were caused by radiation exposure.
How to Heal Your Mouth, Teeth, and Jaw: Reclaim Dental and Orthodontic Health At Home for Kids and Adults
How to Heal Gum Fistula Naturally Using Reactive Oxygen Species Medicine and Photodynamic Therapy
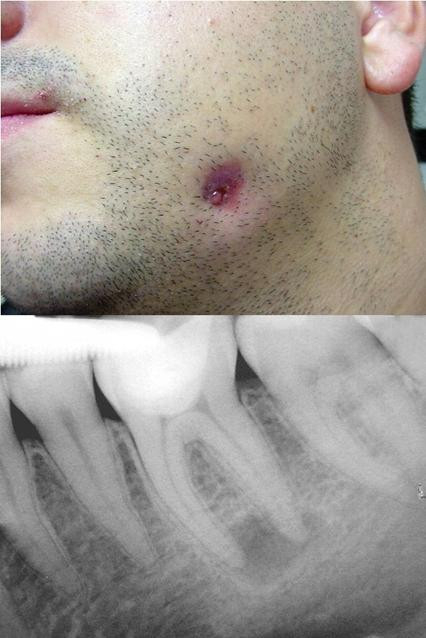
Gum fistulas often open up suddenly without warning. Gum fistulas may be caused by previous dental surgeries and/or infection. Many people wonder, can fistulas heal naturally? If you’ve been going about a normal routine and suddenly you have a gum fistula, you probably would like to avoid dental surgery, if at all possible. But if you have a fistula open up in your gum tissue, this is a sign that there’s an infection. Your body is trying to overcome the infection by draining the infected cavity. You can help this process along by using Reactive Oxygen Species Medicines and (Dimethylsulfoxide) DMSO at home. And yes, it is possible for a fistula to heal naturally.There are several Reactive Oxygen Species Medicines that we talk about in other parts of this discussion, but if you have fistula, it would be ideal to use DMSO combined with either Chlorine Dioxide or Food Grade Hydrogen Peroxide to treat the infection. DMSO has the ability to carry the Chlorine Dioxide and Food Grade Hydrogen Peroxide deep into tissues that may be harboring infection. DMSO can also seek out and destroy infectious pathogens because it is chemically attracted to them and has the ability to easily pass through human cells. Combine Jim Humble’s Dental Health Protocol with the Protocol 1000 PLUS. This is one of most reliable natural ways to heal a fistula that takes shape in the mouth.
Click here to buy food grade hydrogen peroxide 3%.
Natural Ways to Heal a Fistula Due to Radiation Exposure
If you have a fistula anywhere in the body that was caused by radiation exposure, you may benefit from Photodynamic Therapy using Methylene Blue and Red Light Therapy. This is a treatment approach that can be used at home as long as you are NOT taking antidepressant medications (Methlene Blue is an MAOI). If you’re on pharmaceuticals that have been prescribed by a doctor, ask your doctor first before using Methylene Blue to treat a fistula caused by radiation at home.If your doctor does not approve of using Methylene Blue because you’re on prescription medications that could interact negatively with the Methylene Blue, you can still use Red Light Therapy, but pay close attention to your body and only expose the fistula to red light for 5 minutes per treatment session. The effects of red light therapy build up over time causing the cells to become energized. If you expose the radiation fistula to 5 minute Red Light Therapy treatments, you can do these treatments up to 3 times per day.
If you are able to use Methylene Blue as part of your treatment strategy to get a fistula to heal itself, take 1 mg/kg of body weight daily in divided doses. In other words, determine the proper dose for yourself at 1 mg/kg of body weight and then divide that dose in half and administer one half in the morning and one half at night. Shortly after administering the Methylene Blue (wait about 15 minutes ideally), begin shining the red light at the fistula and continuing shining the light at the fistula for about 5 minutes. The red light should be held 1-5 inches away from the skin. The red light reacts with the Methylene Blue in a specific way that energizes the cells to make it easier for the fistula to heal naturally.
Also note that Lugol's iodine supplementation can protect the body from radiation exposure burns. We'll talk more about Lugol's in terms of how it can heal a fistula naturally below.

Click here to buy Lugol's iodine 2%.
How to Heal a Perianal Fistula Naturally
An anal fistula is an infected tunnel that opens up between the skin and the muscular opening (the anal sphincter) at the rectum. According to the Mayo Clinic, anal fistulas typically result from an infection in an anal gland that causes an abscess that spontaneously drains through the skin next to the anus. The fistula is a tunnel that connects the infected gland to the surface of the skin for drainage. But where does the initial infectious pathogen that causes the fistula come from? If you have a perianal fistula, it’s likely that you have other digestive issues that are being caused by the same pathogen.If you have a fistula that opens up in your nether regions that’s not due to radiation, but rather due to infection, consider doing the MRSA Protocol using Chlorine Dioxide Solution or Jim Humble’s Patch Protocol using both Chlorine Dioxide Solution and DMSO. These protocols were specifically designed to be used on drug-resistant bacteria, viruses, or fungi that are not responding to other types of treatment. Note that the MRSA protocol is not just for MRSA, but for drug-resistant infections that are open to the air. You may need help from a trusted friend or family member to do the MRSA protocol if the fistula is in your perineal region, but this is a powerful treatment that works quickly to kill pathogens that cause serious diseases that are not treatable using the drugs your doctor prescribes. Using Chlorine Dioxide Solution, you will mix two substance together to release a gas that goes directly into the fistula. This is Chlorine Dioxide gas (NOT Chlorine gas, as many readers fear—Chlorine Dioxide gas is not nearly as toxic as Chlorine gas, though you should follow the Gas Lung Protocol precisely if you wish to use this gas to treat lung tissues.) and when it is released into a wound that is resistant to antibiotic treatment, it rapidly kills the infectious pathogens and often, the abscess drains immediately.

Click here to learn more about the CDS / MMS Protocols Database.
Can antibiotics heal a fistula?
The treatment recommendations for patients who go to a doctor to heal a perianal fistula or anal fistula include the following:- Antibiotic therapy
- Metronidazole
- Ciprofloxacin
- Biologic agents
- Immunomodulators
- Bile Acid Sequestrants (to treat chronic diarrhea)
- Cholestyramine
- Colestipol
- Colesevelam
- Surgery
- Draining the abscessed anal gland and cutting setons
- Endorectal advancement flap treatment
- Laser surgery
- Video-assisted surgery
- Endoscopic surgery
- Endoscopic fistulotomy
- Endoscopic clipping
- Adult mesenchymal stem cell therapy
These treatments for fistula all involve serious side effects and very little hope of actually being able to heal a fistula without surgery. Why? Because most patients who have developed a fistula have inflammatory bowel diseases such as ulcerative colitis or Crohn’s disease and if antibiotics and other conventional medicine treatment have not already cured these diseases, then there is little hope that conventional medicine will be able to heal a fistula without surgery. Indeed, even with surgery, the anal fistula may return if the offending pathogen that is causing Crohn’s disease, ulcerative colitis, or other digestive issues is not removed from the body. Surgery can weaken the immune system and it can also weaken the tissues surrounding the fistula in some cases. If you feel like surgery is not the right choice for you, consider giving Reactive Oxygen Species Medicine and perhaps Photodynamic Therapy a try first for 3 to 4 weeks and then re-evaluate.
Abdominal Fistulas: How is Enterocutaneous Fistula treated?
An enterocutaneous fistula is an abnormal tunnel that develops between the intestinal canal and the stomach or sometimes between the intestinal tract and the skin. It is sometimes known as an abdominal fistula. This particular type of fistula is especially serious, so if you’re looking for a cure for enterocutaneous fistula, there are certain things that you need to know about Reactive Oxygen Species Medicines and Dimethylsulfoxide (DMSO) and how to use these medicines to heal an intestinal fistula naturally. Reactive Oxygen Species Medicine and DMSO can also be used at home to foster faster healing after enterocutaneous fistula surgery.Click here to buy DMSO 99.9% pharmaceutical grade.
What is the best cure for a fistula?
Reactive Oxygen Species Medicines are one of the natural ways to heal a fistula. Though many people have a hard time viewing Chlorine Dioxide Solution or Food Grade Hydrogen Peroxide as “natural” substances, the fact is, when you take these substances or use them medicinally, they work by releasing singlet oxygen species into the body which are, in fact, produced naturally by the human body to cure infection. Singlet oxygen species, in fact, have an enormous range of action against bacteria, viruses, fungi, and just about any other type of pathogen that might infect the body. This is why we regard Reactive Oxygen Species Medicines as the best cure for a fistula, including abdominal fistulas.Reactive Oxygen Species Medicines include the following:

Click here to buy Artemisia annua / Qing Hao.
How to Cure a Fistula Naturally
In order to fully understand why Reactive Oxygen Species Medicine could work as a cure for enterocutaneous fistula, you need to understand what causes enterocutaneous fistula in the first place. A fistula is caused by infection and it’s likely, if you have an abdominal fistula, that you’ve experienced other serious digestive issues such as inflammatory bowel disease. Enterocutaneous fistula and most other abdominal and perianal fistulas happen in patients who have been diagnosed with Crohn’s disease or ulcerative colitis. Both of these diseases are caused by pathogens that have colonized the liver, the gallbladder, or the pancreas leading to severe digestive problems. Conventional medicine does not recognize these diseases as “infectious”, but rather as “autoimmune” or “genetic” which means, basically, that patients cannot hope for a cure. But both Crohn’s disease and ulcerative colitis can, in fact, be cured using Reactive Oxygen Species Medicines along with Dimethylsulfoxide (DMSO).Click here to learn more about how to heal Crohn's disease naturally as well as ulcerative colitis.
How to Use Reactive Oxygen Species Medicines and DMSO for Treating Abdominal Fistula
You can combine DMSO with Reactive Oxygen Species Medicine. DMSO is an FDA approved medicine that has the broadest medicinal action of any substance currently listed in the pharmaceutical index though doctors rarely use it because it is not promoted by Big Pharma. But DMSO has a toxicity level similar to that of water. It can be used by pregnant women, lactating women, infants, and young children. And it can easily be combined with either Food Grade Hydrogen Peroxide or Chlorine Dioxide to potentiate these medicines and ensure that they reach the right location in the body.Patients can gain access to both Reactive Oxygen Species Medicines as well as DMSO for use at home. Reactive Oxygen Species Medicines like Chlorine Dioxide can be used alongside conventional medicine treatments if patients are afraid to go against their doctor’s orders, but these medicines should not be taken within 30 minutes of taking pharmaceuticals and they should not be taken within 30 minutes of food or supplements either.
On the other hand, if you wish to use DMSO as a treatment for enterocutaneous fistula, you have several options. If you aren’t taking prescription medications, you can add DMSO to your Reactive Oxygen Species Medicines to strengthen their effects and ensure that they find their way directly to the infection. DMSO has a chemical structure that causes it to be attracted to pathogens. But DMSO also has the special ability to heal human tissues. Combining this substance with Reactive Oxygen Species Medicines is a powerful cure for enterocutaneous fistula.
Reactive Oxygen Species Medicines, in contrast, have been studied for their effects against infectious pathogens that cause fistulas and other inflammatory bowel disease issues and they work through various mechanisms. First of all, this class of medications has the ability to kill a wide range of different pathogens, but because singlet oxygen species (which are released by Reactive Oxygen Species Medicines) are produced naturally in the body to work, at times, as “messengers” between cells, this type of medicine alerts the immune system to the presence of ailing human cells, causing these cells to be discarded while simultaneously providing extra oxygen for new, healthy cells to grow.
Chlorine Dioxide and DMSO can both be administered intravenously as well as by mouth or they can be applied to the skin. Patients who are able to ingest the Chlorine Dioxide and DMSO and take them by mouth may start with the Protocol 1000 PLUS. Patients, on the other hand, who are not able to take in food or drink by mouth could use the Protocol 3000 which involves putting Chlorine Dioxide Solution on the skin with DMSO as a skin penetrant. DMSO has the ability to open human cells and it easily passes through the skin carrying whatever is mixed with it. This medicine can be applied all over the body to prevent sepsis due to intestinal fistula while also encouraging the body to heal by sending singlet oxygen signals to the immune system alerting it to the fact that there is an infection and there are unhealthy human cells that need to be removed and replaced. Additionally, if you cannot eat, or if you recently had surgery to repair an enterocutaneous fistula, you could use the MMS Patch Protocol on the surface of the skin where the abdominal fistula is located to hasten the healing process.
Be aware that DMSO can cause the skin to become very dry. Add water if you develop redness in the treatment site.
How to Heal Enterocutaneous Fistula Due to Radiation Treatment
If you developed an enterocutaneous fistula due to radiation treatment, you should know that DMSO can protect the body from the effects of radiation and can help heal tissues that have been exposed to radiation. In some cases, a mixture of 50% hexane free castor oil and 50% DMSO applied topically may be used with red light therapy to encourage the tissues to heal. Red light therapy using a light in the red to infrared spectrum has the ability to re-energize human cells that have been exposed to radiation.Rectovaginal Fistula Treatment and Vesicovaginal Fistula Treatment
Rectovaginal fistulas (abnormal tunnels between the rectum and the vagina) and vesicovaginal fistulas (abnormal tunnels between the vagina and the bladder) may be caused by birth trauma, pre-existing Crohn’s disease or ulcerative colitis, radiation treatment, or perineal lacerations. Often these fistulas involve the sphincters in the pelvic region. Doctors typically recommend surgery as a treatment for vesicovaginal fistula or rectovaginal fistula.Rectovaginal fistula and vesicovaginal fistula have been treated with light therapy in clinical settings. Patients who are not able to afford this type of treatment in a hospital setting or who wish to heal a fistula naturally should consider the use of both Reactive Oxygen Species Medicines and DMSO that we’ve discussed above along with a very different type of treatment that works through opposing mechanisms in the body. Methylene Blue and Red Light Therapy can be used to heal a fistula without surgery in some cases. In rectovaginal fistulas or vesicovaginal fistulas that were caused by birth trauma or laceration of the tissue, Methylene Blue and Red Light Therapy may not work to heal fistula openings because the tissues may have already healed into a tunnel and may need to be reopened through surgery to repair the problem. However, in situations involving the presence of an infection that makes it impossible for a fistula to heal on its own, Methylene Blue and Red Light Therapy may be useful as part of a therapeutic process that would need to be “cycled” with Reactive Oxygen Species Medicines in order to be effective.
The reason why you would need to use Reactive Oxygen Species Medicines for a period of time followed by the use of Methylene Blue and Red Light Therapy (otherwise known as Photodynamic Therapy) is because Methylene Blue cancels out the effects of Reactive Oxygen Species Medicines.
Essentially, this treatment approach would involve the use of red light administered directly into the vagina for 5 to 15 minutes after taking a dose of Methylene Blue (dosing is administered as 1 mg per kg of body weight). The Methylene Blue then goes into the blood stream and reacts with the red light to re-energize cells that may be ailing due to exposure to radiation or infectious pathogens.
If you have an infection that is causing a rectovaginal fistula or a vesicovaginal fistula, follow the Protocol 1000 PLUS along with the MMS Douche Protocol for 3 weeks prior to using Methylene Blue and Red Light Therapy to re-energize cells. This two-pronged treatment approach that begins with Reactive Oxygen Species Medicine with DMSO followed by Methylene Blue and Red Light THerapy can be beneficial for women as they are awaiting surgery as a way to invigorate the cells and encourage fast healing after surgery.
Obstetric Fistulas
Obstetric fistulas are among some of the most severe type of birth injury that can occur during labor. I first became aware of this type of birth injury when I was hired by a government agency to write a white paper for doctors in a U.S. state with one of the highest maternal mortality rates. My boss wanted me to write an educational piece to alert doctors to birth injuries that occurred regularly in this state along with signs and symptoms of these injuries. As I did research into obstetric fistulas, I found that most articles that talk about this type of birth injury in English make sure to mention the idea that women in developed countries rarely have to worry about obstetric fistulas. But I could recall at least one woman in Kansas who’d given birth to twins who developed a large rectovaginal fistula and described her trauma to me in great detail. So this supposedly “rare” situation was not so rare that I didn’t know anyone who had ever had the problem (and had been willing to discuss it with me). And it certainly wasn’t rare at all in the state that had hired me to write a white paper for doctors to help them pay heed to women who described their birth injury symptoms in the hopes that they’d receive proper care.So let’s talk about obstetric fistulas. There are four different types of obstetric fistula listed below:
- Vesicovaginal fistula - an abnormal passage between the bladder and the vagina
- Rectovaginal fistula - an abnormal passage between the rectum and the vagina
- Urethrovaginal fistula - an abnormal passage between the urethra and the vagina
- Vesicouterine fistula - an abnormal passage between the bladder and the uterus
Obstetric fistulas in developed countries such as the U.S. tend to occur due to negligence of hospital staff or because of prolonged or obstructed labor. I had a friend who spent 28 hours in labor because her doctor wanted to delay delivery of her baby until after the new year. This poor woman underwent attempted suction and forceps delivery with a 3-way episiotomy that went all the way from her vagina down to her anus before the doctor finally did a C-section. She was too poor to sue him for damages and the trauma of her delivery stayed with her for decades. This type of negligence can result in the development of a fistula due to tissue death in the vagina. It can be slow to heal if doctors don’t know how to treat it or diagnose it properly.
In undeveloped countries, an obstetric fistula may develop because women are too far away from a health facility and labor and delivery is delayed. If the baby is poorly positioned and the head puts too much pressure on vaginal walls, tissues may die. But women in developed countries can experience similar delays if they live some distance from a hospital or even if they go to a hospital, but they receive poor medical care which is more common than the healthcare industry would like to admit. Nonetheless, women all over the world, in both poor and rich countries may develop an obstetric or gynecological fistula due to any of the following:
- Prolonged or obstructed labor
- Rape
- Accidental injury during surgery
- Unsafe abortions
- Radiation therapy
- Predisposing disease such as Crohn’s Disease or other type of inflammatory bowel disease
It is estimated that 50,000 to 100,000 new cases of obstetric or gynecological fistula happen each year. Again, it is hard to find an honest discussion about obstetric or gynecological fistulas as they pertain to women in developed countries who lack access to quality and compassionate healthcare because the healthcare industry has become so focused on greed and capitalistic pursuits. A number of web sites talk about how women who develop obstetric fistulas in impoverished countries experience depression, isolation, and increased poverty as well as trauma, but I would argue that women in developed countries experience a similar set of issues.
In this discussion, we talk about viable treatments for obstetric fistulas and gynecological fistulas. Most doctors in the developed world recommend surgery for women with obstetric fistulas, but we will focus on alternative treatments for complex cases of obstetric fistula as well as at-home treatment options for women who do not have access to healthcare. We will also discuss options for women who have tried a number of different treatment options for a fistula that simply refuses to heal.
Stem Cell Treatment for Obstetric Fistulas
Adipose-derived stem cells have been used to safely close Crohn’s disease fistula in women who wish to have additional children. Researchers have used stem cells to close obstetric fistulas as well. In one study, patients received 2 doses of 20 million and 40 million cells every 3 to 4 months or 6.6 million and 20 million adipose-derived stem cells every 9 months. The rectovaginal fistulas and vesicovaginal fistulas healed and these patients then went on to successfully birth additional, healthy children.Mesenchymal stem cell treatments from adipose tissue are administered locally at the site of the birth injury.
Individuals with Crohn’s Disease are more susceptible to the development of a perianal fistula during childbirth. Anal fistula is a common problem even in men with Crohn’s Disease. Both men and women with Crohn’s Disease might consider the use of Chlorine Dioxide and / or Dimethylsulfoxide (DMSO) as a way to cure Crohn’s Disease. Women with Crohn’s can benefit from the use of Chlorine Dioxide and DMSO prior to childbirth to cure Crohn’s Disease. Both of these medicines are safe for use during pregnancy.
Fistulizing Inflammatory Bowel Disease and Obstetric Fistulas
Patients who already have an inflammatory bowel disease such as Crohn’s disease may develop obstetric fistulas that are difficult to treat. Indeed, patients with Crohn’s Disease may be prone to developing rectovaginal fistulas even without pregnancy or a birth injury. The most common causes of a rectovaginal fistula in Crohn’s patients include surgical mistakes or an infection in the rectum. The standard conventional medical treatment for fistula in patients with Crohn’s or other inflammatory bowel disease includes the following:- Antibiotic therapy
- Immunomodulators
- Anti-tumor necrosis factor - alpha drugs
- Placement of setons
- Placement of a Diverting Stoma
- Surgery (often using a “surgical flap” procedure)
The use of stem cells to treat rectovaginal fistulas in patients with Crohn’s Disease has a success rate between 60 to 88%. Stem cell treatments along with surgical intervention often works to heal anal fistuals even if patients have had prior unsuccessful surgeries. Stem cells are typically injected after surgery is complete. Stem cell types that are implanted to treat both anal fistulas caused by Crohn’s Disease as well as obstetric fistulas caused by birth injury include the following:
- Stromal vascular fraction stem cells
- Autologous expanded adipose-derived stem cells
- Allogenic adipose-derived stem cells.
Note that all of these stem cell types are derived from the patient’s own fat cells. Some patients receive repeated doses of stem cells during the healing process after fistula surgery. Patients who do not fully heal from the surgery and stem cell treatments typically still experience some progress toward healing even if the fistula does not close entirely.
No adverse effects have been reported for stem cell therapies and surgery for rectovaginal fistula.
Photodynamic Therapy for Vesicovaginal Fistula, Rectovaginal Fistula, Urethrovaginal Fistula, and Vesicouterine Fistula
Photodynamic Therapy is a type of treatment that involves the use of a photosensitizing agent along with light of a specific wavelength that activates the photosensitizer, making it into a medicine. The term “photodynamic therapy” sounds very technical which tends to scare patients off from doing this type of therapy at home. But, in fact, our bodies are designed for this type of medicine. A good example of a powerful Photodynamic Therapy treatment that uses sunlight is Artemisia annua treatment. Artemisia annua is an herb that was used in Tanzania as the treatment-of-choice for COVID-19. The use of Artemisia annua made it possible for Tanzania to stay somewhat immune to COVID-19 for much of the pandemic (that is, until the country changed presidents). Artemisia annua releases molecules of hydrogen peroxide into the body that are “cleaved” into singlet oxygen species when the body is exposed to sunlight. These singlet oxygen species have an extremely broad spectrum of action in the body and have the ability to cure a wide variety of infectious diseases from viruses and bacteria to parasites and fungi. The use of Artemisia annua with sunlight exposure is technically a type of “photodynamic therapy” that people can easily use to overcome disease at home. An obstetric fistula or an anal fistula caused by birth injury or due to Crohn’s Disease or an inflammatory bowel condition can be treated with photodynamic therapy. Doctors have used 5-aminolevulinic acid 2% along with fiber optic lasers in the red light spectrum to heal obstetric fistula as well as anal fistula caused by Crohn’s Disease or other inflammatory bowel disorders. About 2 hours after the 5-aminolevulninic acid 2% is injected into the area around the fistula, a red light is shined into the vagina or anus. This causes the release of a singlet oxygen species. There were no negative side effects reported using this treatment method and it has a success rate of approximately 80%. This particular treatment cannot be performed at home, but it nonetheless demonstrates the potential value of using photodynamic therapy to heal an obstetric fistula caused by Crohn’s Disease. Patients can do a modified version of Photodynamic Therapy using Methylene Blue and Red Light Therapy as discussed above.Methylene Blue is an over-the-counter pharmaceutical that is readily absorbed by rectal tissues that also responds to exposure to red light and infrared light wavelengths.

Click here to buy Methylene Blue.
Lugol's Iodine and Vitamin K2 / MK-7 to Heal a Fistula Naturally
Most people who come to us for health coaching are iodine and vitamin K2 deficient. These nutrient deficiencies are extremely common in the modern world and we generally recommend the Lugol's iodine protocol for those who wish to heal a fistula naturally. If you aren't yet familiar with vitamin K2 as a bone and tooth healing medicine, click here to read more about this nutrient.
Click here to buy vitamin K2 / MK-7.
Lugol's iodine is such an important nutrient and it plays such a big role in human health that we wrote over 400 pages about it. If you have a fistula that won't heal, you may want to learn a bit about this nutrient and why it might help your body overcome the downward spiral. Iodine, like vitamin K2, is a nutrient that has been systematically removed from food supplies all around the world.
Lugol's iodine supplementation along with the supportive nutrients and trace minerals can help bring dead or near-dead cells back to life while promoting proper immune system function. That's why you need it in order to heal a fistula! If you live in a developed nation, chances are, you're deficient in this vital nutrient. Click here to read about how and why iodine and vitamin K2 were removed from the food supply in developed nations and the role of organophosphates and GMO foods in this process.
Click here to buy Lugol's iodine 2%.

Click here to buy The Iodine Bible.
Resources: