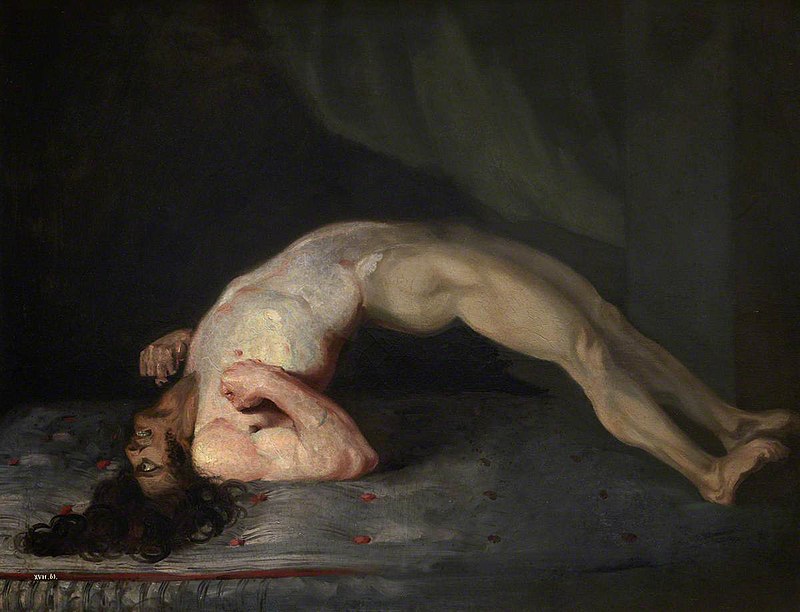How to Prevent Rabies and Tetanus Following an Animal Bite or Injur
NOTE: Click here to read about how to cure flesh-eating bacteria disease / gangrene / necrotizing fasciitis.
How to Prevent Tetanus or Rabies At Home
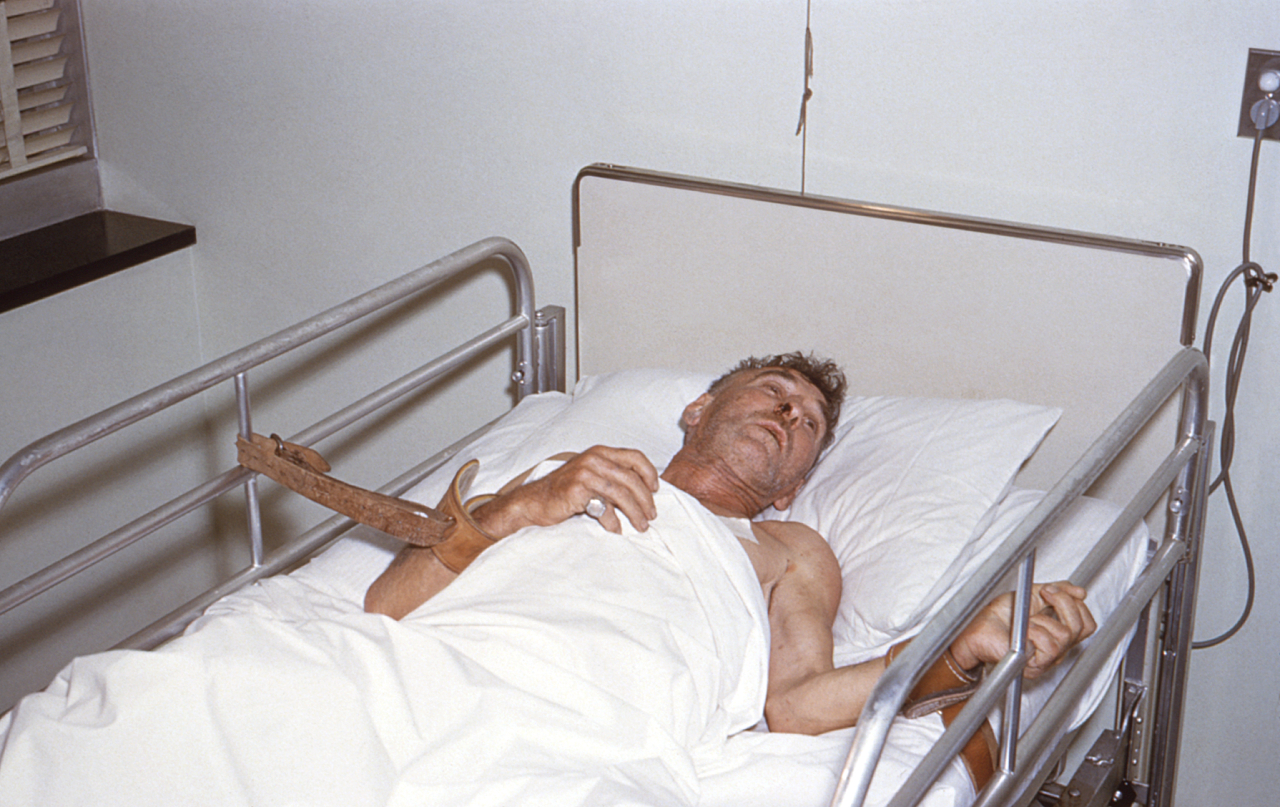
If you are exposed to Tetanus or Rabies via a bite from an animal or if you are exposed to tetanus as a result of an accident, or through a wound that involved rusty metal, you should begin the Tetanus Protocol as soon as possible. This disease has an incubation period of 3 to 7 days. The sooner you begin the Emergency Rabies / Tetanus Protocol, the less likely that you’ll experience the severe and painful muscular contractions that are caused by the tetanus pathogen or the excess salivation, heart arrhythmias, or breathing abnormalities caused by rabies.Both Rabies and Tetanus are deadly infections that must be addressed immediately, ideally before symptoms begin. If you have been exposed to rabies or tetanus while traveling in a foreign country and you don’t have access to these vaccines or if you don’t want to get vaccinated, you will need to begin rabies / tetanus treatment at home immediately. You should enlist someone’s help if symptoms of these diseases have already set in.
 Click here to sign up for the CDS Protocols App!
Click here to sign up for the CDS Protocols App!
Preventing a Cytokine Storm
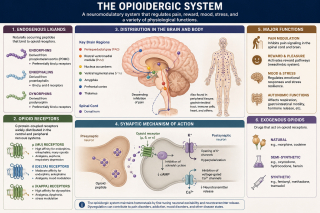
Patients who have been bitten by an animal or who have gotten a wound from a metal object should take 500-1500 mg of vitamin B3 (Nicotinamide or Niacin) daily in divided doses to suppress the production of pro-inflammatory cytokines due to infection. Begin taking vitamin B3 in high doses as soon as possible after the initial exposure to rabies / tetanus.
Emergency Rabies Treatment: Rabies Prevention After Being Bitten by an Animal
Rabies is a disease that is caused by a virus. This disease is very different from tetanus in that the incubation period is anywhere from 1 week to 1 year with an average of 2 to 3 months. Once symptoms of rabies begin, neurological damage is almost certain and as such, early treatment is very important. Some people do survive rabies even without Chlorine Dioxide treatment, but the death rate from this disease is extremely high.Few people have had a rabies vaccine in either the developed or the undeveloped world, but rabies is a serious issue particularly for travelers and individuals living in less developed regions of the world. Anyone who has been bitten by an animal should consider following the pre-symptom tetanus protocol that we describe below for at least 14 days.
If rabies symptoms develop at any time during the initial 14 day treatment, switch to Protocol 3000 and the Spray Bottle Recipe if patients are not able to ingest fluids. Rabies symptoms kill victims by compromising the brain’s ability to control salivation, breathing, and heartbeat.
Click here to buy Chlorine Dioxide Solution for humans with the hydrochloric ccid activator.
CDS / MMS Protocol If Tetanus Symptoms Have Not Yet Appeared:
Malaria Protocol:
If symptoms of tetanus have already begun to appear, follow the malaria protocol through 3 doses of 18 activated drops according to the schedule outlined in the Malaria Protocol chapter. If you know when the exposure to tetanus occurred, and you have completed the malaria protocol, begin the Protocol 1000 PLUS and continue with this protocol until 10 days have passed since the tetanus exposure.Use enemas consisting of filtered water to cleanse the digestive system of toxins during treatment.
Protocol 1000 PLUS:
After you have completed the Malaria Protocol, wait for 6 to 8 hours and begin the Protocol 1000 PLUS. Be sure to do enemas to cleanse the digestive system as you work through these protocols. Continue with the Protocol 1000 PLUS until 10 days have passed since the tetanus exposure.If symptoms of tetanus appear, move on to Protocol 3000 and obtain the assistance of a loved one to assist with the application of this Protocol and the Spray Bottle Recipe.
Sea Water Supplementation:
Super-hydrate the body with sea water supplements if you have not yet developed symptoms of tetanus yet. Take 2 tablespoons of sea water in 8 ounces of purified water three times per day.Click here to learn more and subscribe to the Living Database now.
CDS / MMS Protocol If Tetanus Symptoms Have Already Appeared:
If symptoms of tetanus have already appeared, expect to administer Protocol 3000 and the Spray Bottle Recipe continuously for 10-12 hours continuously. After 10-12 hours of treatment, if the patient is responding well to the treatment, switch to high-dose vitamin C treatment administered until the patient begins to experience diarrhea (which signifies that he/she has reached the maximum limit of vitamin C that can be absorbed by the digestive system).Protocol 3000
If tetanus symptoms have already appeared, administer Protocol 3000 hourly. On the half hour, administer the MMS1 Spray Bottle Recipe.
Spray Bottle Recipe
Administer the Spray Bottle Recipe continuously over the entire body whenever you are not administering Protocol 3000.
Click here to schedule a health coaching session with us.
High Dose Vitamin C
After 10-12 hours of continuous MMS / CDS treatment, administer 6 to 8 grams of vitamin C (6000-8000 mg). The patient should develop diarrhea from this treatment. Begin by administering 4 grams / 4000 mg of vitamin C. Administer an additional 1 gram / 1000 mg of vitamin C hourly until the patient develops diarrhea.High Dose Vitamin C is an appropriate treatment once the patient has clearly overcome the most serious symptoms of the disease. An antioxidant like vitamin C can help prevent tissue damage due to an over-production of oxidants.

The CDS / MMS Book Bundle - Learn About Chlorine Dioxide, Dimethyl Sulfoxide, and Complementary Therapies for Both Medicines. PURCHASE THE BUNDLE HERE!
Resources: