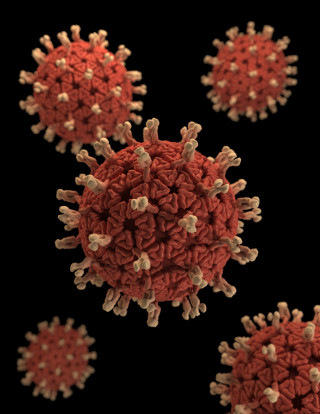
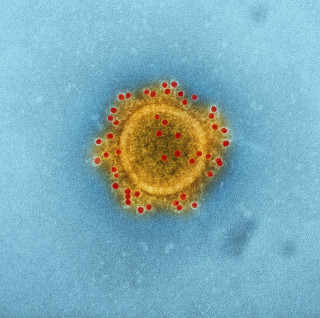
Why You Need to Understand Cytokine Storm Syndrome to Cure COVID...
 IMPORTANT NOTE: Scientists have recently realized that COVID-19 (as well as many respiratory infections) need to be treated in 2 phases. Phase 1 takes place during the first 2-3 days of acute infection when symptoms are not that severe. During this initial phase of infection, treatment with Reactive Oxygen Species medicines like Chlorine Dioxide are appropriate to lower the viral load. However, treating the infection with Reactive Oxygen Species medicines like Chlorine Dioxide beyond this initial 2 to 3 day window could worsen symptoms. During Phase 2 of the infection, when coughing begins, it is vital to supplement with Vitamin B3 at no less than 1000 mg per day (500 mg in the morning and 500 mg in the evening). Patients should also be given medicines to counteract the effects of a cytokine storm during this stage. We provide a list of potential options that you can use to treat a cytokine storm at home at this link.
IMPORTANT NOTE: Scientists have recently realized that COVID-19 (as well as many respiratory infections) need to be treated in 2 phases. Phase 1 takes place during the first 2-3 days of acute infection when symptoms are not that severe. During this initial phase of infection, treatment with Reactive Oxygen Species medicines like Chlorine Dioxide are appropriate to lower the viral load. However, treating the infection with Reactive Oxygen Species medicines like Chlorine Dioxide beyond this initial 2 to 3 day window could worsen symptoms. During Phase 2 of the infection, when coughing begins, it is vital to supplement with Vitamin B3 at no less than 1000 mg per day (500 mg in the morning and 500 mg in the evening). Patients should also be given medicines to counteract the effects of a cytokine storm during this stage. We provide a list of potential options that you can use to treat a cytokine storm at home at this link.
Consider using a Methylene Blue, Vitamin C, and NAC protocol for Phase 1 treatment and then continue with Methylene Blue through Phase 2 for COVID-19.
Cytokine Storm Basics
A cytokine storm is classified as an inflammatory syndrome and is (put simply) an over-exaggerated immune response. This condition is formally known as “hypercytokinemia” and generally occurs after a person is infected with a pathogen. Then, the immune system kicks into action by producing cytokines and other immune proteins to fight the infection. The production of cytokines is normal and expected, however when the immune system starts to produce too many cytokines, or continues to produce them even after the pathogen has been defeated, this is where the problems start. In fact, in many COVID-19 cases (or in other coronavirus cases), most deaths or severe health issues following the disease are caused by the effects of cytokine storm rather than by the infection itself. Of course, this can be confusing, since it’s possible for the COVID-19 infection and the cytokine storm syndrome to exist simultaneously.In cytokine storms, the particularly high levels of cytokines and other proinflammatory immune proteins circulating in the blood provoke inflammation not only in areas of the body where there are pathogens, but also in other areas of the body. And, with cytokine storm, the body doesn’t stop producing these proinflammatory agents after the pathogen is destroyed. The immune system continues to produce proinflammatory immune proteins even after the infection is gone (in normal situations, the body stops producing these particular proteins once the pathogen is successfully destroyed). Thus, chronic inflammation occurs. Chronic inflammation in the body like that which is seen during a cytokine storm can lead to severe tissue damage and even organ failure in severe cases, as we’ll look at below.
Some common symptoms of a cytokine storm include (but are not limited to):
- Fever (present in nearly all cases)
- Fatigue
- Anorexia
- Headache, muscle pain, and joint pain
- Rash
- Diarrhea
- Some neuropsychiatric issues
In addition, a lot of individuals experiencing a cytokine storm also have respiratory symptoms such as coughing or rapid breathing, which when left untreated can sometimes even lead to ARDS (acute respiratory distress syndrome). In particularly severe situations, renal failure and liver injury, along with cardiac issues, may also occur. 7 Other signs of cytokine storm include an enlarged spleen, low counts of all types of red blood cells, white blood cells, and platelets, excessive bleeding, and multiple organ failure. 4
One thing that’s important to keep in mind with cytokine storm is that it can either exist simultaneously with an infection (such as COVID-19), or it can exist independently after the infection has been treated. This is what makes the concept of cytokine storm so confusing for many people. Even after treating a COVID-19 infection successfully, some people still have uncomfortable or threatening symptoms, and these symptoms often happen to mimic the symptoms of COVID-19 itself (meaning that it can be difficult to tell whether you’ve successfully recovered from the infection or not).
Normally, the immune system is supposed to return to a state of homeostasis after fighting off an infection. When your body is first exposed to the pathogen, it sends out cytokines and other immune cells to wage war against the pathogen. Some amount of inflammation occurs in the body as part of this normal immune response. After the pathogen has been defeated, however, the immune cells (including inflammatory cytokines) are supposed to return to a dormant state, awaiting the next pathogen exposure. In a cytokine storm, the body’s rules for returning to normal after an infection are overridden. For example, an extreme pathogen load or a long period of immune activation (such as following a persistent infection) can lead to a cytokine storm.
In order for an overactive immune response to officially be considered a cytokine storm, it must meet the following conditions:
- There are elevated cytokine levels circulating in the blood
- There are significant signs of systemic inflammation (this includes symptoms such as chronic pain, gastrointestinal issues, mood disorders/anxiety/depression, fatigue, etc.)
- Either the patient shows signs of secondary organ dysfunction (generally in the kidneys, liver, or heart) unrelated to an existing pathogen, OR the patient has organ dysfunction completely driven by cytokine-related inflammation and action.
Cytokines are not inherently bad. We need our immune cells to produce cytokines in order to successfully fight infection. However, overproduction or prolonged production of cytokines is negative for inflammatory tissues and organs. When this happens, it’s necessary to calm one’s immune response in order to be able to recover (first you calm your immune response, and then you can heal damaged tissues and begin recovery, especially in the case where you’ve already gotten rid of the invading pathogen). 1
In the development of cytokine storms, researchers have found that there are two specific cytokines that contribute to the damage incurred: tumor necrosis factor alpha (TNF-alpha) and interferon-gamma (IFN-gamma). These cytokine proteins have been found to be primarily responsible for organ failure and COVID-19-like symptoms that occur after the disappearance of an actual COVID-19 infection. While indeed there are many different kinds of pro-inflammatory proteins that may be present in higher quantities in the bodies of people with a cytokine storm, these two particular cytokines are directly related to the potentially fatal effects of cytokine storm. 2 Another cytokine protein known as interleukin-6 (IL-6) can also be a major contributor in the onset of a cytokine storm. 3
Together, the TNF-alpha and IFN-gamma cytokines cause inflammatory cell death, a process whereby normally healthy cells “explode”. When nearby immune cells see this, they respond by secreting more cytokine proteins, which then go on to cause cell death in even more cells, therefore fueling the storm. The medicines and therapies listed below help stop the production of these cytokines and some also inhibit the ability of these cytokines to “recruit” other immune cells to produce more pro-inflammatory agents. 2
When a cytokine storm starts, it’s necessary to calm the immune system effectively in order to bring the patient back to health. Read more about natural treatments used to treat cytokine storms at this link.

Related Posts:
Resources: